New 2026 Cholesterol Guidelines: What Cardiologists Now Recommend (and How to Apply It in Daily Life)
If you’ve ever stared at your cholesterol lab report wondering what those numbers really mean—or worried whether you’re doing enough to protect your heart—you’re not alone. With heart disease still the leading cause of death, the new 2026 cholesterol guidelines from leading US cardiologists are a big deal, and they’re designed to make prevention clearer and more personal than ever.
In this guide, you’ll find what’s actually changed in the latest recommendations, how to understand your LDL, HDL, and triglycerides in plain language, and what practical steps—medications, lifestyle changes, and follow-up testing—make the biggest difference for lowering your risk of heart attacks and strokes.
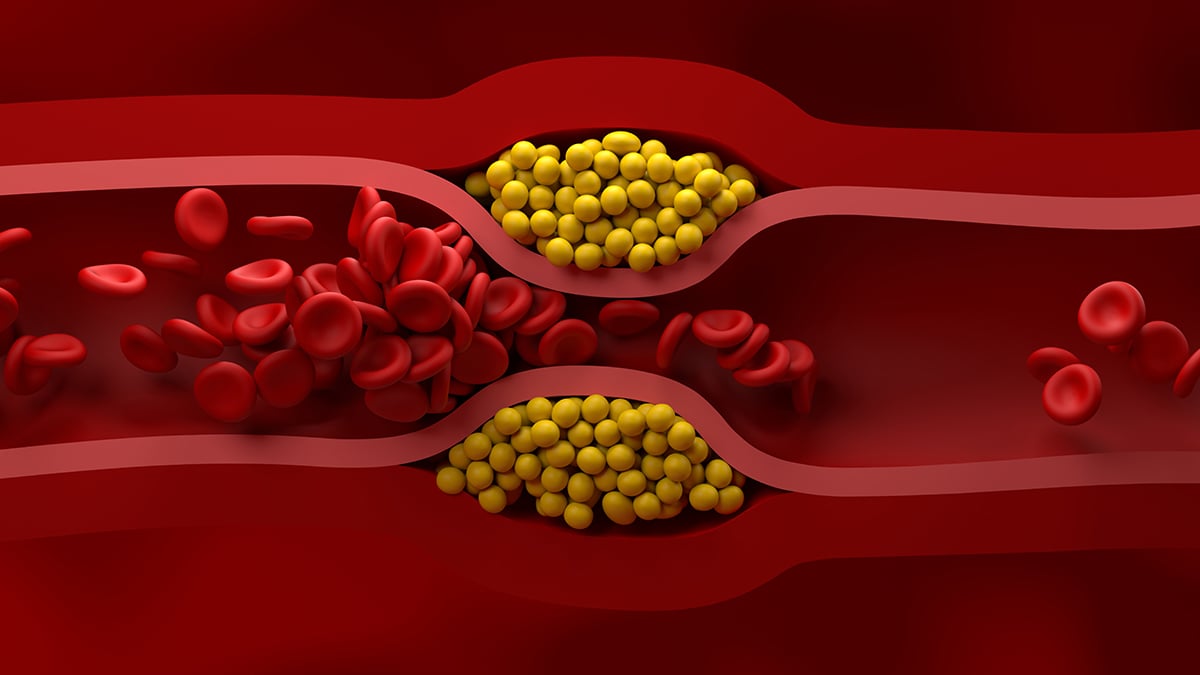
Why New Cholesterol Guidelines Matter in 2026
The updated cholesterol guidelines—developed by expert panels of US cardiologists and published in early 2026—respond to several realities:
- Heart disease and stroke remain top causes of death, despite better treatments.
- Many people at high risk still aren’t on cholesterol-lowering therapy.
- Newer medications and more precise risk tools can now tailor treatment.
- Evidence keeps growing that earlier and more aggressive LDL lowering in high‑risk people prevents events.
“Every 1 mmol/L (about 39 mg/dL) reduction in LDL cholesterol leads to roughly a 20–25% reduction in major cardiovascular events over time. The new guidelines lean into this principle—especially for people at highest risk.”
The goal isn’t to put everyone on pills. Instead, the guidelines push for a smarter mix of:
- Understanding your personal risk.
- Making strong lifestyle changes that actually fit your life.
- Using medications when the benefit clearly outweighs the risk.
Making Sense of Your Cholesterol Numbers in Light of the New Guidance
While exact cutoff values can vary slightly by organization, the new guidelines keep the same basic message: lower LDL (“bad” cholesterol) is better, especially if you’re at high risk.
Key lab values and what they generally mean
- LDL-C (low-density lipoprotein)
Often called “bad” cholesterol because it contributes to plaque in arteries.
Guideline direction: focus on how low you can reasonably go, depending on risk category, rather than a one-size-fits-all “normal.” - HDL-C (high-density lipoprotein)
The “good” cholesterol that helps remove excess cholesterol from blood. Extremely high levels are not always better, but low HDL is often a marker of higher risk and unhealthy lifestyle factors. - Triglycerides
A type of blood fat linked with diet, obesity, and diabetes. Very high levels raise pancreatitis risk; moderately high levels often travel with metabolic syndrome. - Non-HDL cholesterol
Total cholesterol minus HDL; increasingly used as a broader marker of “atherogenic” particles.
The 2026 guidance leans more heavily on overall cardiovascular risk (age, blood pressure, smoking, diabetes, kidney disease, family history, and sometimes coronary artery calcium scores) than on cholesterol numbers alone.
What’s New in the 2026 US Cholesterol Guidelines?
While the core principles from earlier guidelines (like the 2018 ACC/AHA recommendations) remain, several themes have been strengthened or clarified based on recent research.
1. Even stronger emphasis on LDL lowering in very high‑risk people
- People with established cardiovascular disease (prior heart attack, stroke, stent, or bypass) are urged to reach very low LDL levels if tolerable.
- Combination therapy (statin + ezetimibe, or adding a PCSK9 inhibitor) is highlighted when statins alone don’t get LDL “low enough” for these patients.
2. More personalized risk assessment tools
- Risk calculators are being updated with more diverse population data.
- Role of coronary artery calcium (CAC) scoring is reinforced to clarify decision‑making for people at “borderline” or “intermediate” risk.
3. Expanded roles for non‑statin therapies
Recent trials have shown that certain add‑on drugs further reduce events when LDL is still not controlled on statins:
- Ezetimibe – a well‑studied oral add‑on that lowers LDL modestly.
- PCSK9 inhibitors – injectable drugs (like evolocumab or alirocumab) that can dramatically lower LDL, now backed by more long‑term data.
- Bempedoic acid – an oral option that can help, particularly for some people who cannot tolerate higher‑dose statins.
The new guidelines clarify where these medications offer the most benefit, typically in:
- Very high‑risk patients who cannot get LDL low enough on statins alone.
- People with familial hypercholesterolemia (genetic very high cholesterol).
- Patients who are truly statin‑intolerant after careful evaluation.
4. Greater attention to triglycerides and metabolic health
Elevated triglycerides, especially in people with diabetes or metabolic syndrome, are getting more attention, with emphasis on:
- Weight loss, physical activity, and reduced added sugars and alcohol.
- Considering high‑dose purified omega‑3 (such as icosapent ethyl) in select high‑risk patients, based on prior trial data.
Lifestyle First: Daily Habits That Align With the New Guidelines
Medications can be powerful, but the new cholesterol guidelines still put heart‑healthy lifestyle at the foundation. The difference now is an emphasis on realistic, sustainable changes—not perfection.

1. Heart‑healthy eating patterns
Instead of obsessing over single “superfoods,” the guidelines focus on dietary patterns such as:
- Mediterranean-style diet – vegetables, fruits, whole grains, beans, nuts, olive oil, and fish.
- DASH-style diet – emphasizes produce, low‑fat dairy, lean proteins, and less sodium.
Practical steps you can start with:
- Fill half your plate with vegetables at most lunches and dinners.
- Swap refined grains (white bread, pastries) for whole grains (oats, brown rice, quinoa).
- Use olive oil or canola oil instead of butter for most cooking.
- Eat fatty fish (like salmon, sardines) 1–2 times per week, if possible.
- Limit processed meats, sugary drinks, and deep‑fried foods to occasional treats.
2. Movement and physical activity
The guidelines align with broader cardiovascular recommendations:
- Aim for at least 150 minutes per week of moderate‑intensity activity (like brisk walking) or 75 minutes of vigorous activity, if you’re able.
- Add 2 days of resistance training (body‑weight, bands, or weights) to preserve muscle and support metabolism.
3. Weight, sleep, and stress
- Even a 5–10% weight loss in people with overweight or obesity can noticeably improve triglycerides and other risk factors.
- Sleep of 7–9 hours per night, with evaluation for sleep apnea when indicated, is tied to better cardiometabolic health.
- Chronic stress can worsen blood pressure, eating habits, and inflammation—mindfulness, therapy, community, and boundaries can all help.
Medications: How the New Guidelines Recommend Using Statins and Beyond
For many people at moderate to high risk, lifestyle alone isn’t enough to reduce risk to safe levels. The guidelines continue to place statins as the cornerstone of therapy, supported by decades of data.
1. Who is most likely to be recommended a statin?
- Adults with established cardiovascular disease (secondary prevention).
- People with LDL ≥ 190 mg/dL, often indicating familial hypercholesterolemia.
- Adults aged roughly 40–75 with:
- Diabetes, or
- Intermediate to high 10‑year ASCVD risk on a validated calculator.
2. Clarifying statin safety and side effects
Muscle aches and concerns about liver health or diabetes often cause people to stop statins. The new guidance reinforces:
- True serious side effects are uncommon.
- Most mild symptoms can be managed by:
- Lowering the dose.
- Trying a different statin.
- Using alternate‑day dosing in select cases.
- The reduction in heart attacks and strokes usually far outweighs the small increase in blood sugar or other risks for most high‑risk patients.
Many patients stop statins after hearing a story from a friend or social media. When we review the actual evidence together, quite a few feel more comfortable re‑trying a lower dose or a different statin—and their numbers and risk improve dramatically.
3. When non‑statin medications enter the picture
The guidelines support adding or substituting other agents when:
- LDL remains above target in very high‑risk patients on maximally tolerated statins.
- A patient is truly unable to tolerate any reasonable statin regimen.
Choice of medication takes into account cost, insurance coverage, side effect profiles, and how much additional LDL reduction is needed.
Common Obstacles—and Realistic Ways to Overcome Them
Knowing the guidelines is one thing. Living them is another. Many people struggle with time, motivation, side effects, or just feeling overwhelmed. The new guidance implicitly acknowledges this by encouraging shared decision‑making and stepwise change.
Obstacle 1: “I don’t have time for a heart‑healthy lifestyle.”
- Batch‑cook simple, heart‑healthy meals on weekends.
- Schedule short walks into your calendar like appointments.
- Use grocery delivery or pre‑chopped produce if that’s feasible and reduces friction.
Obstacle 2: Fear or experience of medication side effects
- Keep a symptom diary when starting or changing a medication.
- Discuss trial periods of different statins and doses with your doctor.
- Ask if blood tests (like CK or liver enzymes) are appropriate if you’re worried.
Obstacle 3: Conflicting information online
The guidelines encourage clinicians to help patients separate high‑quality evidence from anecdotes or marketing. Look for:
- Information from major cardiology societies or academic centers.
- Clear references to randomized trials and long‑term outcome data.
- Balanced discussion of benefits and risks, not miracle claims.
A Step‑by‑Step Plan to Apply the New Cholesterol Guidelines With Your Doctor
You don’t need to memorize the full guideline document. Here’s a practical way to put its core ideas into action.
- Get an updated, fasting (or non‑fasting, as advised) lipid panel.
Ask your clinician whether fasting is necessary in your case and how often your levels should be checked. - Review your overall cardiovascular risk.
Discuss age, blood pressure, smoking status, family history, diabetes, kidney disease, and any prior events. Ask if a risk calculator or coronary artery calcium scan could clarify your risk level. - Agree on a realistic lifestyle plan.
Choose 1–2 specific, achievable changes (for example, “20‑minute walk after dinner 4 nights per week” or “vegetables at lunch every weekday”). - Decide together about medications.
If your risk is high enough for medication, ask:- What benefit can I expect over the next 5–10 years?
- What side effects should I watch for?
- When will we re‑check labs and follow up?
- Plan follow‑up.
Put your next lab test and appointment on the calendar before you leave, so adjustments can be made based on real data.

Before and After: What Change Can Look Like (Without Overpromising)
Results vary from person to person, and no guideline can guarantee that a heart attack or stroke will never happen. But studies consistently show meaningful risk reductions when LDL is lowered and lifestyle improves.
Before applying guideline-based care
- LDL: 150 mg/dL
- Inconsistent exercise
- Frequent fast food and sugary drinks
- Unclear understanding of personal risk
- No statin, despite intermediate–high risk
After 12–24 months of guideline-based care
- LDL reduced to < 70 mg/dL with statin ± ezetimibe
- Regular walking routine most days
- More home‑cooked, plant‑forward meals
- Clear follow‑up plan and lab monitoring
- Substantially lower estimated 10‑year risk of heart attack or stroke
Moving Forward: Turn the New Guidelines Into Your Personal Heart‑Health Plan
The new 2026 cholesterol guidelines don’t change the basic truth that has been clear for years: lowering harmful cholesterol—especially LDL—reduces the risk of heart attacks and strokes. What’s new is how precisely and personally those recommendations can now be applied.
You don’t need to fix everything overnight. The most powerful thing you can do this week is to take one concrete step:
- Schedule a visit or telehealth check‑in to review your latest labs.
- Ask your clinician directly: “Based on the latest guidelines, what is my risk, and what would you recommend I focus on first?”
- Choose a small, specific lifestyle change you’re willing to try for the next month.
Over time, these choices add up. With a combination of informed medical care and sustainable daily habits, you can align your life with the best evidence we have today—and give your heart the long‑term support it deserves.
Further Reading and Trusted Resources
For more detailed, clinician‑level information, these reputable sources regularly publish and update cholesterol management guidance:
