How a Common Acne Antibiotic Turned One Woman’s Skin Jet Black—and What You Need to Know
When a woman started a routine antibiotic to calm her rosacea, she expected a clearer, calmer face—not to wake up weeks later with her arms and legs turning a striking shade of black. A recent case report highlighted by Gizmodo describes how a standard treatment with minocycline, a commonly used antibiotic for skin conditions, triggered dramatic hyperpigmentation that left her limbs looking like something out of a medical horror movie.
While her story is unsettling, it offers something important: a chance to understand a rare but real side effect, so you can spot warning signs early, ask better questions, and make safer decisions about antibiotics for acne, rosacea, and other skin problems.
The Case: When Rosacea Treatment Took a Dark Turn
According to the case report described in early April 2026, the woman began taking minocycline, a tetracycline-class antibiotic often prescribed for:
- Rosacea flare-ups
- Moderate to severe acne
- Certain bacterial infections involving the skin
Within about two weeks of starting therapy, she developed dramatic, dark discoloration of her limbs. Photographs published with the report show her arms and legs with patchy, almost ink-black pigmentation, while other areas of her body remained relatively spared.
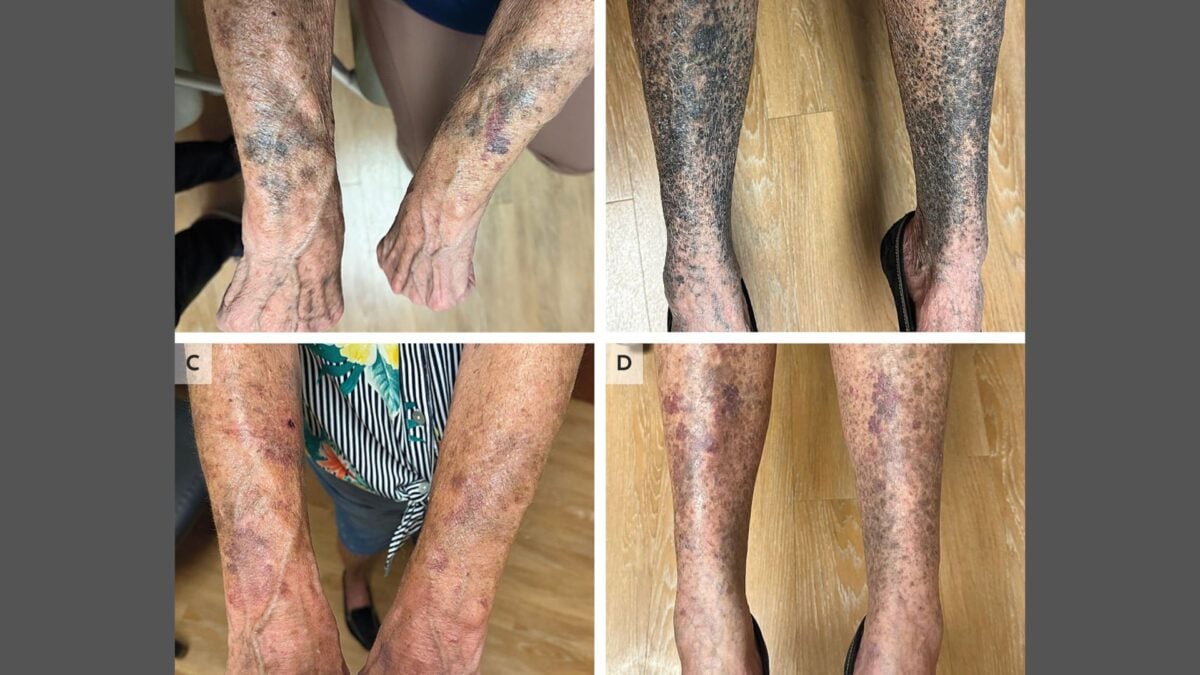
Once doctors linked the pigment changes to minocycline, they stopped the drug and worked to manage her symptoms. Hyperpigmentation from minocycline can fade after discontinuation, but in some cases, it can take months—or even remain partially permanent.
“This kind of reaction is uncommon, but not unheard of. The key is recognizing it early and re‑evaluating whether the antibiotic is still the right choice for that patient.” — Dermatologist commentary on minocycline reactions
What Is Minocycline and Why Is It Used for Skin Conditions?
Minocycline is an oral antibiotic in the tetracycline family. Dermatologists have used it for decades because it:
- Reduces acne-related bacteria on the skin
- Helps calm inflammation, which is key in rosacea
- Can be taken for weeks to months when needed under supervision
Compared with older tetracyclines, minocycline penetrates tissues well and has convenient dosing, which is why it became a go‑to for chronic skin issues. However, its benefits come with a known list of possible side effects, including:
- Gastrointestinal upset (nausea, stomach pain)
- Dizziness or vertigo
- Autoimmune-like reactions in rare cases
- Drug-induced lupus in some long-term users
- Hyperpigmentation—darkening of skin, nails, or even internal tissues
Minocycline-Induced Hyperpigmentation: What Actually Happens?
Hyperpigmentation simply means “increased pigment.” With minocycline, it’s more complex than a typical tan or post-acne mark. The drug can form complexes with iron or other molecules and deposit in skin and other tissues, creating dark staining.
Dermatologists usually describe three main types of minocycline hyperpigmentation:
- Type I: Blue-grey spots, often in acne scars or inflamed areas (like the face)
- Type II: Blue-grey patches on normal skin, especially the shins and forearms
- Type III: More diffuse brown discoloration on sun‑exposed areas
The case highlighted by Gizmodo appears especially dramatic, with large areas of dark staining on the limbs—visually closer to the more extensive Type II or Type III patterns.

Evidence from dermatology studies suggests that:
- Hyperpigmentation risk increases with higher cumulative doses and longer duration of use.
- People with inflammatory skin disease may be more likely to develop it in affected areas.
- Some individuals may have a genetic predisposition to pigment changes, though this is still being studied.
Early Warning Signs to Watch For
If you are taking minocycline—or a loved one is—it’s important not to panic, but to watch for gradual changes. Hyperpigmentation often starts subtly.
Signs that warrant a conversation with your prescriber include:
- New blue-grey or brown spots in old acne scars or areas of previous inflammation
- Patchy darkening on the shins, forearms, or hands
- Unusual dark streaks or staining on the nails
- Darkening of gums or inside the mouth
- Any widespread skin color change that doesn’t match normal tanning
Who Is Most at Risk for This Side Effect?
Hyperpigmentation from minocycline is still considered uncommon, but certain patterns increase the likelihood:
- Long-term use (many months or years)
- Higher total dose over time
- Use for chronic conditions like acne or rosacea rather than short infections
- History of easy pigment changes from other medications
- Extensive sun exposure without protection
Skin tone also changes how hyperpigmentation looks. On lighter skin, grey or blue discoloration may be more obvious. On darker skin, it may present as deeper brown or almost black areas that can easily be mistaken for other pigment conditions.
“Anytime we put someone on long-term minocycline, we talk frankly about pigment risks and schedule follow‑ups. Most patients still choose to use it—but now they know exactly what to look for.” — Board‑certified dermatologist
If Your Skin Starts to Darken: What Doctors Typically Do
The first and most important step in suspected minocycline hyperpigmentation is usually stopping the medication, in partnership with your prescriber. Do not discontinue any prescription abruptly without consulting your clinician, but don’t delay bringing up changes either.
Management often includes:
- Clinical evaluation: A dermatologist or prescribing clinician examines the pattern, timing, and severity of pigmentation.
- Medication review: They check for other drugs or supplements that might contribute to pigment changes.
- Alternative treatment planning: For acne or rosacea, they may adjust to:
- Different oral antibiotics with lower pigment risk (e.g., doxycycline in some cases)
- Topical therapies (metronidazole, azelaic acid, ivermectin, or retinoids)
- Non‑antibiotic systemic options if needed
- Sun protection: Broad‑spectrum sunscreen and protective clothing to prevent further darkening of affected areas.
- Monitoring and possible procedures: Over months, pigment may gradually lighten. For persistent areas, dermatologists sometimes consider laser or light‑based treatments, although results vary.

Safer Strategies: Treating Acne and Rosacea Without Over‑Relying on Antibiotics
One of the key lessons from this case is that our default approach to skin disease still leans heavily on chronic antibiotics—sometimes longer than necessary. For many people, there are effective alternatives that reduce long‑term drug exposure.
For rosacea, evidence‑based options include:
- Topical metronidazole, azelaic acid, or ivermectin
- Low‑dose doxycycline (sub‑antimicrobial dosing) in some cases
- Laser or light therapies for visible blood vessels and redness
- Lifestyle strategies: trigger avoidance (heat, alcohol, spicy foods), gentle skincare, and daily sunscreen
For acne, consider:
- Topical retinoids (adapalene, tretinoin, etc.)
- Benzoyl peroxide combinations to reduce bacterial resistance
- Hormonal therapy in appropriate patients (e.g., certain oral contraceptives, spironolactone)
- Short, targeted courses of antibiotics with a clear stop date
Understanding Outcomes: Hyperpigmentation Before and After Treatment
Everyone wants to know: “Will it go away?” The honest answer is: not always completely, and usually not quickly.
Clinical experience and published case series suggest a rough pattern:
- Early, mild pigment changes may fade significantly over 6–12 months once minocycline is stopped, especially with sun protection.
- Longstanding or very dark staining can persist for years and may only partially improve.
- Laser treatments can help selected patients but are not guaranteed and can be expensive.

The woman in the 2026 report is still a single case, and details on her long-term outcome are limited. What we can say is that early recognition and discontinuation generally improve the chances of partial or significant fading over time.
How to Talk With Your Doctor About Antibiotic Skin Treatments
Conversations about risk can feel intimidating, especially when you’re desperate for relief from painful or embarrassing skin symptoms. A few prepared questions can make the discussion more balanced and collaborative.
Consider asking:
- “What are the potential short‑ and long‑term side effects of this antibiotic, including skin discoloration?”
- “How long do you expect me to stay on it, and what is the criteria for stopping?”
- “What non‑antibiotic options could we try first or combine with this?”
- “How often should we check in to monitor for side effects?”
- “What should I look for at home that would warrant a call or visit?”

What the Research and Experts Say
The reaction described in Gizmodo’s article is rare, but it aligns with decades of dermatology literature on minocycline. Published reviews have estimated clinically noticeable hyperpigmentation in a minority of long‑term users, particularly at higher cumulative doses.
Key evidence‑based points include:
- Minocycline is effective for many inflammatory skin diseases, but it carries unique pigment and autoimmune risks compared with some alternatives.
- Hyperpigmentation risk rises with dose and duration, though some cases—like this one—can occur surprisingly early.
- Shorter courses and non‑antibiotic strategies can often achieve similar control with fewer long‑term consequences.
For more detailed scientific reviews, see open‑access summaries from dermatology journals and professional societies such as:
Staying Informed Without Living in Fear
The images from this woman’s case are hard to look at—and they’re meant to be. They remind us that even familiar medications can have serious, if uncommon, side effects. But they should lead to informed vigilance, not panic.
If you’re using or considering minocycline for rosacea, acne, or another skin condition, you don’t have to navigate the trade‑offs alone. You can:
- Ask candid questions about benefits, risks, and alternatives.
- Check your skin regularly and photograph any new discoloration.
- Use daily sun protection to limit pigment changes from any cause.
- Speak up early if something doesn’t look or feel right.
You deserve clear explanations and a treatment plan that respects both your appearance and your long‑term health. Let this unsettling story be a prompt—not to avoid helpful medicines outright—but to use them wisely, with your eyes wide open and your care team fully engaged.
If you’re currently on minocycline and notice new or unusual skin darkening, schedule a visit with your prescriber or a dermatologist. An early conversation now can spare you from bigger problems later.
