Why Measles Outbreaks Are Costing America Millions — And What We Can Do Now
Measles was once so rare in the United States that most younger doctors had never seen a case. Yet by early 2026, the country had already recorded more than 1,000 infections, with outbreaks stretching from West Texas to communities across the Southeast and beyond. The human cost is obvious: sick children, worried parents, and overworked health workers. But behind the headlines is a quieter story — one of mounting financial strain, disrupted lives, and a public health system being pushed to its limits.
This page breaks down what’s really happening with measles outbreaks in the U.S., what they cost in dollars and in lives, and—most importantly—what practical, evidence-based steps you can take to protect your family and your community without getting lost in fear or misinformation.
The Measles Comeback: What’s Happening in 2025–2026?
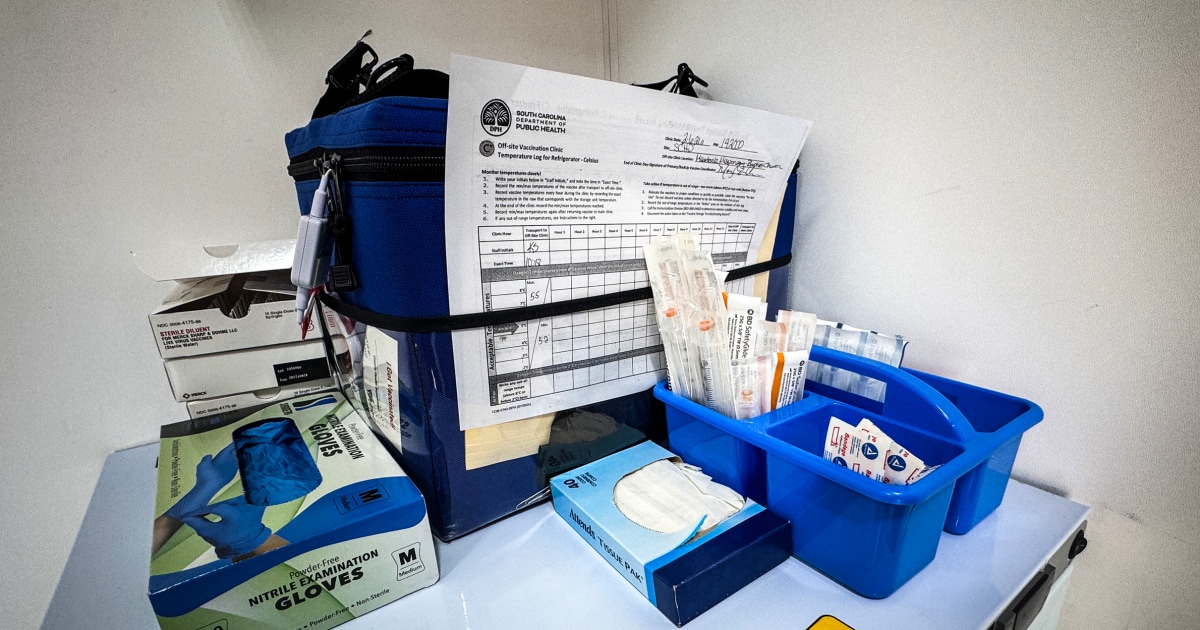
According to recent reporting from NBC News and public health agencies, the U.S. has already seen more than 1,000 measles cases in 2026, building on a sharp rise that began in 2024 and 2025. In early 2025, for example, an outbreak in West Texas forced local health departments to rapidly mobilize staff, secure emergency funding, and coordinate across county lines—all while trying to reassure anxious parents.
These aren’t isolated events. Clusters have emerged in areas where vaccination rates have slipped below the roughly 95% coverage needed for herd immunity. Once measles finds a pocket of unvaccinated children or adults, it spreads with almost ruthless efficiency.
- One person with measles can infect up to 9 out of 10 unvaccinated people they come into close contact with.
- The virus can linger in the air for up to two hours after an infected person leaves a room.
- People are contagious before they even realize they’re sick, which makes containment harder and more expensive.
“Measles is so contagious that if one person has it, up to 90% of the people close to that person who are not immune will also become infected.”
— U.S. Centers for Disease Control and Prevention (CDC)
The Hidden Price Tag: How Much Do Measles Outbreaks Really Cost?
When people hear that “measles outbreaks are costing the U.S. millions of dollars,” it can sound abstract. But for health departments, hospitals, schools, and parents, those costs are very real—and they add up fast.
1. Direct Medical Costs
Not every measles case requires hospitalization, but when it does, the bills can be steep. Studies of past outbreaks in the U.S. have found that:
- Hospitalized measles patients can generate tens of thousands of dollars in charges per case, especially if intensive care is needed.
- Even outpatient visits require lab tests, isolation rooms, personal protective equipment, and follow-up care.
2. Public Health Response Costs
Public health departments bear one of the biggest financial burdens. During an outbreak, they must:
- Identify and contact potentially exposed people (sometimes hundreds per case).
- Organize emergency vaccination clinics.
- Coordinate with schools, childcare centers, and workplaces.
- Run communication campaigns to counter misinformation.
Analyses of previous U.S. outbreaks have estimated that:
- Local outbreak responses can cost from tens of thousands to over a million dollars per event, depending on size and duration.
- Per-case public health costs have ranged from roughly $7,000 to more than $20,000 when intensive tracing and control measures are needed.
3. Lost Productivity and Community Disruption
These are the “true losses” that are hardest to count, but they may be the largest:
- Parents missing work to care for sick children or stay home during quarantine.
- Businesses losing staff unexpectedly, especially in small communities.
- Schools and childcare centers excluding unvaccinated children for weeks, disrupting learning and family routines.
- Delayed medical care for other conditions when clinics are overwhelmed or reconfigured to manage infection risk.
In West Texas in 2025, for example, public health officials had to shift staff away from routine services to focus almost entirely on measles—leaving fewer resources for chronic disease management, maternal health, and other critical programs.
Why Are Measles Cases Rising Again? The Science Behind the Surge
Measles isn’t new, and neither is its vaccine. What has changed is the level of protection in some communities. Several factors have converged:
- Falling vaccination rates: Even small drops below about 95% coverage can open the door to outbreaks.
- Pandemic-related disruptions: During the Covid-19 pandemic, many children missed routine well-child visits and vaccines.
- Misinformation: Persistent myths about vaccine safety, often amplified online, have eroded trust for some families.
- Global travel: Measles remains common in many parts of the world; travel can reintroduce the virus into under-immunized U.S. communities.
“Despite a safe and cost-effective vaccine being available, measles remains one of the leading causes of death among young children globally.”
— World Health Organization
Scientific reviews from organizations like the CDC, WHO, and multiple independent research groups continue to find that the measles-mumps-rubella (MMR) vaccine is highly effective and has a strong safety record. The risk of serious complications from measles—such as pneumonia, brain swelling (encephalitis), or even death—remains far higher than the risk of severe vaccine side effects.

A Closer Look: What an Outbreak Feels Like on the Ground
To understand the true impact of measles, it helps to look beyond national statistics and listen to people managing outbreaks locally. In early 2025, as measles spread through parts of West Texas, local health leaders suddenly found themselves juggling urgent competing needs.
One health director described having to rapidly request emergency funds, reassign staff from chronic disease work to contact tracing, and set up evening vaccination clinics so working parents could bring in their children. Phone lines were jammed with calls from worried families asking whether it was still safe to send kids to school or daycare.
“We weren’t just treating measles cases—we were trying to keep the rest of the health system functioning while answering hundreds of questions from the community. Every hour spent on this outbreak was an hour we couldn’t spend on other critical services.”
— Local public health official, West Texas (paraphrased from media reports)
Families also felt the strain. Parents of exposed but not yet sick children sometimes faced mandatory quarantine, meaning missing work without guaranteed pay. Schools had to exclude unvaccinated students during the outbreak period, disrupting learning and social support—especially where families already faced financial or childcare challenges.
Evidence-Based Ways to Protect Your Family and Community
While no health decision is completely risk-free, decades of data give us a clear picture: high measles vaccination coverage dramatically reduces outbreaks, hospitalizations, and deaths—and saves money for families and communities alike. Here’s how to translate the science into practical steps.
1. Make Sure Vaccinations Are Up to Date
- Children: In the U.S., the standard schedule recommends two doses of MMR—first at 12–15 months, second at 4–6 years.
- Teens and adults: Many adults who received two childhood doses are still protected. Those unsure of their status can:
- Ask their healthcare provider to review records.
- Get a blood test to check immunity in certain cases.
- Receive an MMR dose if records are missing and measles risk is high, per provider guidance.
2. Talk Openly With a Trusted Clinician
If you have questions or worries about measles or the MMR vaccine, you’re not alone. Many parents feel caught between conflicting information online. A good pediatrician, family doctor, or nurse practitioner should:
- Listen to your specific concerns without judgment.
- Explain risks and benefits in plain language.
- Share data and real-world experience from their own practice.
3. Plan Ahead for Travel and School Requirements
- Check vaccination requirements well before enrolling in school, college, or daycare.
- Review immunization needs several weeks before international travel.
- Ask your child’s school or camp how they handle outbreaks and exclusions for under-vaccinated students.
4. Support Community-Level Prevention
Individual decisions add up. Communities with strong vaccination rates tend to experience:
- Fewer outbreaks.
- Lower public health response costs.
- Less disruption to schools and local businesses.
You can help by:
- Sharing accurate, science-based information from trusted sources (CDC, WHO, local health departments).
- Advocating for easy access to vaccines—walk-in clinics, flexible hours, and low-cost or free options.
- Encouraging respectful, fact-focused conversations about health decisions in your community and online.
Common Obstacles to Vaccination — And Realistic Ways Around Them
Many families want to keep their children safe but run into real-world barriers. Understanding these challenges is essential if we want to prevent costly measles outbreaks without blaming or shaming people.
1. Time and Access
For parents working long or unpredictable hours, getting to a clinic during the day can be tough.
- Look for evening or weekend vaccine clinics, often run by local health departments or community centers.
- Ask if your child’s school or daycare partners with mobile vaccine providers.
- Check if pharmacies in your state offer MMR for older children and adults.
2. Cost Concerns
Many people worry vaccines will be expensive, especially without insurance. In reality:
- In the U.S., the Vaccines for Children program provides free vaccines for eligible kids through participating providers.
- Community health centers and local health departments often offer low- or no-cost options.
3. Fear and Misinformation
Some parents have heard alarming claims about vaccines that are not supported by high-quality evidence. It’s understandable to feel cautious when you’re responsible for a child’s health.
- Ask your clinician which sources they trust and why.
- Look for information that cites multiple independent studies, not just opinions.
- Be wary of content that uses fear-based language or promises absolute certainty—health decisions almost always involve weighing probabilities.

What Policymakers and Communities Can Do to Reduce Outbreak Costs
Preventing costly measles outbreaks isn’t just about individual choices. Policy and system-level decisions play a major role in how protected—or vulnerable—a community becomes.
1. Invest in Local Public Health
Stable funding helps departments respond quickly without robbing other essential services. Effective investments include:
- Hiring sufficient epidemiology and nursing staff.
- Building strong data systems for tracking immunizations and outbreaks.
- Supporting multilingual, culturally sensitive communication teams.
2. Strengthen School and Childcare Immunization Programs
- Keep requirements clear, consistent, and evidence-based.
- Offer on-site or nearby vaccination opportunities at registration and back-to-school events.
- Provide compassionate outreach to families whose children are missing doses.
3. Address Misinformation Proactively
Rather than only reacting during outbreaks, communities can:
- Partner with local faith leaders, educators, and parent groups to share accurate information.
- Develop easy-to-read, translated materials explaining measles risks and vaccine benefits.
- Train clinicians in communication strategies that build trust, especially with hesitant families.
At a Glance: Measles Outbreaks vs. Vaccination Costs
The numbers vary by location and year, but the overall pattern is clear. Here’s a high-level comparison based on analyses of past U.S. outbreaks and vaccine programs:
Measles Outbreak Costs*
- Public health response per case: thousands of dollars.
- Hospitalization per severe case: tens of thousands of dollars.
- Lost work time: days to weeks for affected families.
- School and childcare disruptions: hard to quantify but widespread.
Vaccination Program Costs*
- Cost of MMR dose: modest compared with hospitalization or outbreak response.
- Prevents the majority of measles cases when coverage is high.
- One-time or two-dose schedule protects for years.
- Reduces strain on health systems and families.
*Estimates based on published studies and public health reports; exact numbers vary by region, insurance coverage, and outbreak size.
Moving Forward: Protecting Health, Budgets, and Peace of Mind
Measles outbreaks in 2025 and 2026 are a warning signal: when vaccination rates slip, we don’t just see more illness—we also see rising healthcare bills, overstretched public health systems, and families scrambling to cope with sudden quarantines and school exclusions. The good news is that we already have the tools to prevent most of this.
No decision about health is free of trade-offs, and it’s reasonable to ask hard questions. But decades of data, and the lived experience of communities on the front lines, point in the same direction: maintaining strong measles vaccination coverage is one of the simplest, most cost-effective ways to protect both individual families and the broader economy.
If you’re feeling uncertain or overwhelmed, you don’t need to solve everything today. You can:
- Check your or your child’s vaccination record.
- Schedule a conversation with a trusted healthcare provider.
- Share one reliable resource on measles with a friend or family member.
Small, informed steps like these, multiplied across thousands of households, are what ultimately keep outbreaks—and their multimillion-dollar price tags—from becoming the new normal.

Trusted Resources for Up-to-Date Measles Information
For the latest guidance and data on measles, vaccination, and outbreaks, consider these authoritative sources:
