Measles Is Surging Again: What Every Family Needs to Know in 2026
If it feels like you’re suddenly hearing about measles everywhere, you’re not imagining it. In the first two months of 2026 alone, the United States has seen nearly 1,000 confirmed cases spread across 26 states—a level that has alarmed pediatricians, emergency departments, and public health officials nationwide.
For many adults, measles was something our grandparents talked about, not a disease we expected to worry about in 2026. Yet with experts calling it “unbelievably contagious,” it’s understandable if you’re feeling anxious, especially if you have young children, are pregnant, or live with someone who has a weakened immune system.
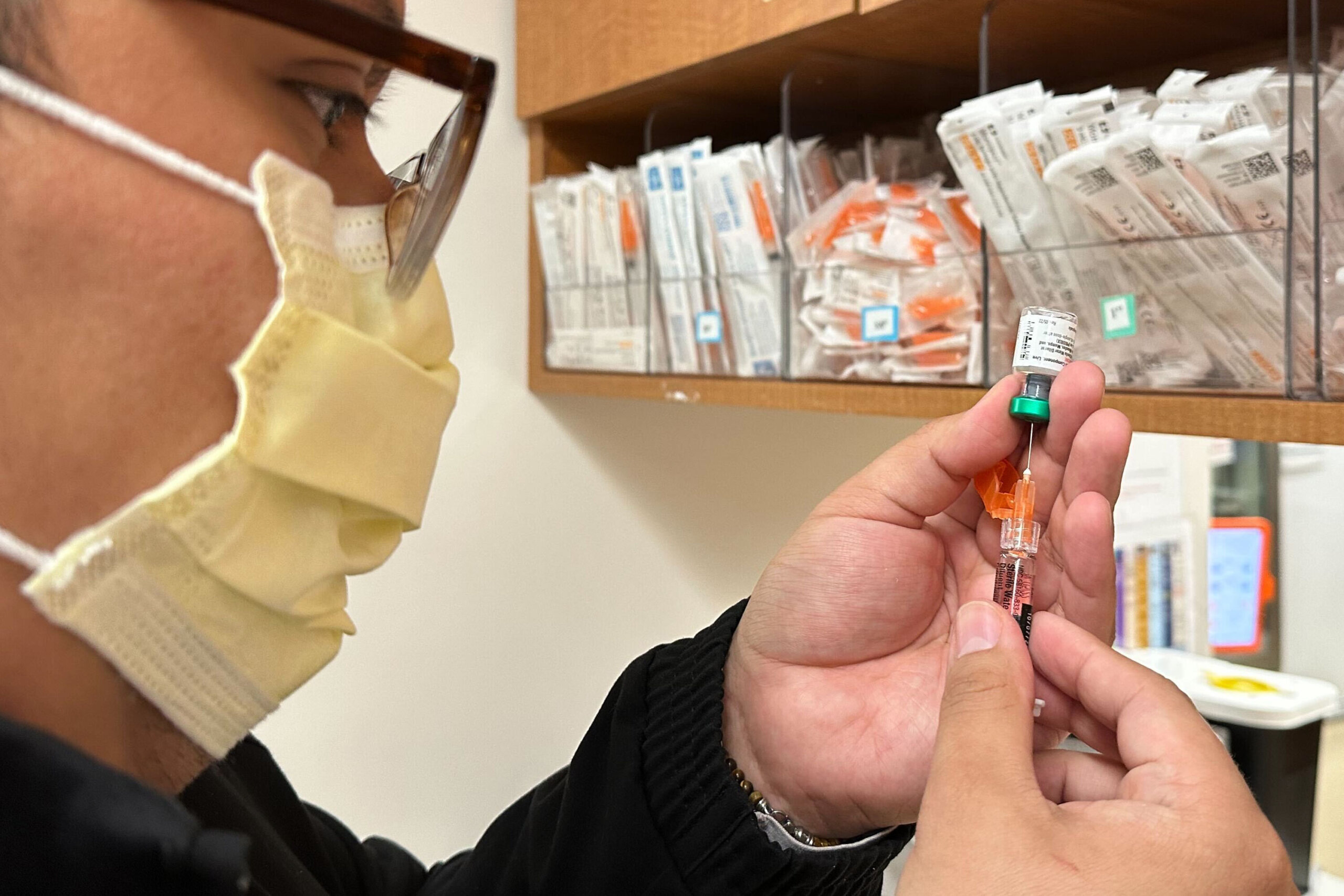
This guide breaks down what you need to know—how measles spreads, what symptoms look like, who is at highest risk, and the most effective ways to protect yourself and your community—using up-to-date evidence and practical, realistic advice.
Measles Cases Are Soaring in 2026: What’s Happening?
According to recent reports, more than 980 measles cases have already been confirmed in the first two months of 2026, across at least 26 states. That’s more than many full years combined in the recent past and represents one of the largest early-year surges in decades.
- Clusters are appearing in communities with lower vaccination rates.
- Cases are linked to both domestic spread and imported infections from international travel.
- Hospitals are reporting increased pediatric admissions and strained emergency departments in certain regions.
“Measles is one of the most contagious viruses we know of. In an unvaccinated group, it can move through a community like wildfire.”
— Infectious disease specialist, university-affiliated medical center
Why Experts Call Measles “Unbelievably Contagious”
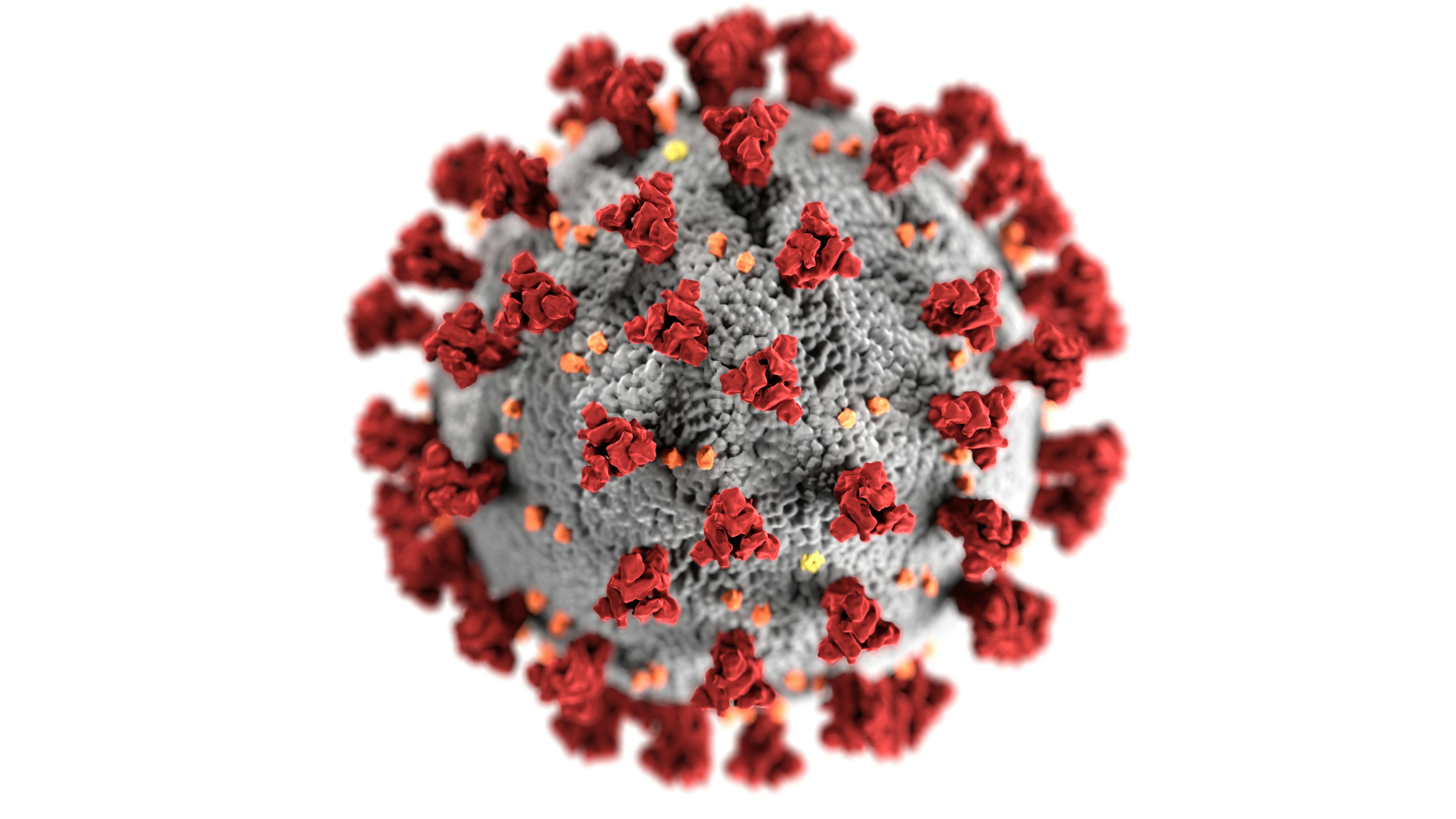
Measles is not “just a rash.” It’s a highly contagious respiratory virus that spreads through the air when an infected person breathes, coughs, or sneezes. Tiny droplets can linger in the air and on surfaces for hours.
Scientists describe measles using the basic reproduction number, or R₀—the average number of people one infected person will infect in a fully susceptible population. Measles often has an R₀ of 12–18, meaning one sick person can infect a dozen or more others if they’re not protected.
- Airborne spread: The virus can remain in the air for up to two hours after a contagious person leaves a room.
- Infectious before rash: People can spread measles about 4 days before the rash appears—before they realize they’re sick.
- High attack rate: Around 9 out of 10 unvaccinated people exposed to measles will become infected.
How to Recognize Measles: Symptoms, Timeline, and Complications
Measles symptoms typically appear 7–14 days after exposure. They often begin like a bad cold and progress to the characteristic rash.
Common early symptoms
- High fever (often 103–104°F / 39.4–40°C)
- Cough
- Runny nose
- Red, watery eyes (conjunctivitis)
- Tiny white spots in the mouth (Koplik spots), usually inside the cheeks
Classic measles rash
The rash usually appears 3–5 days after symptoms begin. It:
- Starts at the hairline and face
- Spreads downward to the trunk, then arms and legs
- Often merges into larger blotches
Possible complications
Most healthy, vaccinated people exposed to measles do not get sick. But for those who are infected—especially young children and adults—the virus can be serious. Reported complications include:
- Ear infections (which can cause hearing loss)
- Pneumonia (a leading cause of measles-related deaths, especially in children)
- Dehydration requiring IV fluids
- Encephalitis (brain swelling), which can cause seizures or long-term neurological problems
- Rare, fatal long-term complication called SSPE (subacute sclerosing panencephalitis), years after infection
Who Is Most at Risk During the 2026 Measles Surge?
Not everyone faces the same level of risk from measles. Some people are more likely to catch the virus, develop complications, or need hospital care.
- Infants under 12 months who are too young for their first routine measles-mumps-rubella (MMR) dose.
- Unvaccinated children and adults, including those who deferred vaccines during the COVID-19 pandemic.
- People with weakened immune systems, such as those receiving chemotherapy, transplant recipients, or individuals with certain immune conditions.
- Pregnant people without documented immunity, due to risks to both parent and fetus.
- International travelers going to regions with active outbreaks if not fully protected.
“We’re especially concerned about babies and immunocompromised patients. They rely on the rest of us being vaccinated to keep the virus from reaching them.”
— Pediatric infectious disease physician
How to Protect Your Family: Vaccination and Practical Steps
The most powerful tool against measles is the MMR vaccine, which protects against measles, mumps, and rubella. Decades of research show it is highly effective and has a strong safety record.
Recommended MMR schedule (in most U.S. guidelines)
- First dose: 12–15 months of age
- Second dose: 4–6 years of age
Two doses are about 97% effective at preventing measles. One dose is about 93% effective.
If you’re unsure about your measles immunity
Many adults are understandably unsure about their vaccination records, especially if they moved, changed doctors, or were vaccinated decades ago. Reasonable steps include:
- Ask your parents or caregivers if they remember your childhood vaccines.
- Contact your pediatrician’s office (if still in practice) or state immunization registry.
- Talk with your current clinician about:
- Getting an MMR booster (safe for most adults who may already be vaccinated).
- Or, in some cases, blood testing (titers) to check immunity.
Beyond the Shot: Everyday Steps to Lower Your Measles Risk
Even with vaccination as the foundation, there are sensible precautions you can take during an outbreak—especially if you have infants or family members who can’t be vaccinated for medical reasons.
- Check local guidance: Follow advice from your local health department or CDC updates about outbreaks in your area.
- Be cautious with travel: If you’re unvaccinated or traveling with infants, discuss measles risk and possible early vaccination with your doctor.
- Review school and daycare policies: Ensure immunization records are up to date; ask how they handle potential exposure.
- If exposed or symptomatic: Call your clinic, urgent care, or ER before going in so they can protect other patients by arranging isolation or alternative entry routes.
- Support high-risk loved ones: Help older relatives or immunocompromised friends avoid crowded indoor spaces in outbreak zones if they’re not fully protected.

Addressing Common Concerns and Vaccine Hesitancy with Compassion
If you’ve had questions or worries about the MMR vaccine, you’re not alone. Many parents feel caught between conflicting information online and a strong desire to do what’s best for their children.
What the evidence shows
- No credible link to autism: Large studies in several countries have found no association between MMR vaccination and autism spectrum disorders.
- Well-studied safety profile: The MMR vaccine has been used for decades worldwide and is continuously monitored for safety.
- Typical side effects: Mild fever, soreness at the injection site, or a brief rash are the most common and usually resolve on their own.
- Serious side effects are rare: Far rarer than the complications associated with actual measles infection.
“I was nervous about vaccines with my first child, too. What helped me was sitting down with our pediatrician, going through the data together, and having space to ask every question without judgment.”
— Parent of two, interviewed during a clinic outreach program
A Real-World Scenario: How One Family Managed a Measles Exposure
In early 2026, a suburban family received a call from their local health department: their 5-year-old had been in the same after-school program as a child later confirmed to have measles.
Here’s how they navigated it, step by step:
- Confirmed vaccination status: They checked their child’s record and confirmed two MMR doses. The health department reassured them the risk of infection was low.
- Monitored for symptoms: For the next 3 weeks, they watched for fever, cough, runny nose, or rash—while the child continued usual activities, since they were fully vaccinated and not sick.
- Protected vulnerable relatives: They postponed a planned visit to an elderly grandparent with lung disease until the incubation period passed.
- Shared accurate information: When other parents in the program became anxious, they shared links from official public health sources instead of social media rumors.
The child never developed measles, which is the most common outcome for fully vaccinated contacts. The experience, though stressful, reinforced for the family how valuable that earlier decision to vaccinate had been.
What a Difference Vaccination Makes: Community “Before and After”
Public health data repeatedly show how quickly measles can accelerate—or fade—depending on local vaccination coverage.


- Before high coverage: One measles case can lead to dozens more, closing schools and stressing hospitals.
- After high coverage: Sporadic imported cases still occur, but they rarely lead to large outbreaks and are easier to contain.
Moving Forward: Calm, Informed Action in a Time of Measles Surge
Measles in 2026 is a real concern, but it’s not a reason to panic. It is a reason to pause, get informed, and take a few concrete steps that can dramatically shift your risk and help protect your community.
To recap, the most impactful actions you can take are:
- Review your family’s MMR vaccination records and schedule any needed doses.
- Talk with your healthcare provider if you’re pregnant, immunocompromised, or planning international travel.
- Stay up to date with local health department or CDC announcements about measles activity in your area.
- Approach friends and family with questions about vaccination with empathy, not judgment, and point them toward reliable sources.
You don’t need to solve the entire measles surge on your own. By protecting yourself and the people around you, you’re contributing to a safer environment for babies, cancer patients, and others who depend on community protection to stay well.
If you haven’t checked your family’s vaccination status recently, consider taking 10 minutes today to do it—that small step can make a profound difference in the weeks and months ahead.
Trusted Resources for Up-to-Date Measles Information
For the latest, evidence-based guidance, consult:
- CDC – Measles (Rubeola)
- World Health Organization – Measles
- Your state or local health department website for outbreak updates and vaccination clinics
- Your primary care clinician or pediatrician for personalized medical advice
