New Global Outbreak Map Reveals Hidden Hotspots: What It Means for Your Health and Travel Plans
Overnight, a new global disease outbreak map can make the world feel a little smaller—and a lot more fragile. When we see bright red “hotspots” spreading across a map, it’s natural to wonder: Is my region next? Is it safe to travel? What can I actually do about this?
A recent global modeling study, highlighted by Earth.com, estimates that about 9.3% of the world’s land area is now considered highly vulnerable to dangerous disease outbreaks. Many of these hotspots are clustered in parts of Latin America and Oceania, regions with rich biodiversity but also complex social and health challenges.
In this guide, we’ll unpack what this new outbreak-risk map really shows, why certain areas are especially vulnerable, and—most importantly—how you can use this information to make calmer, smarter decisions about your health and travel, without slipping into panic.
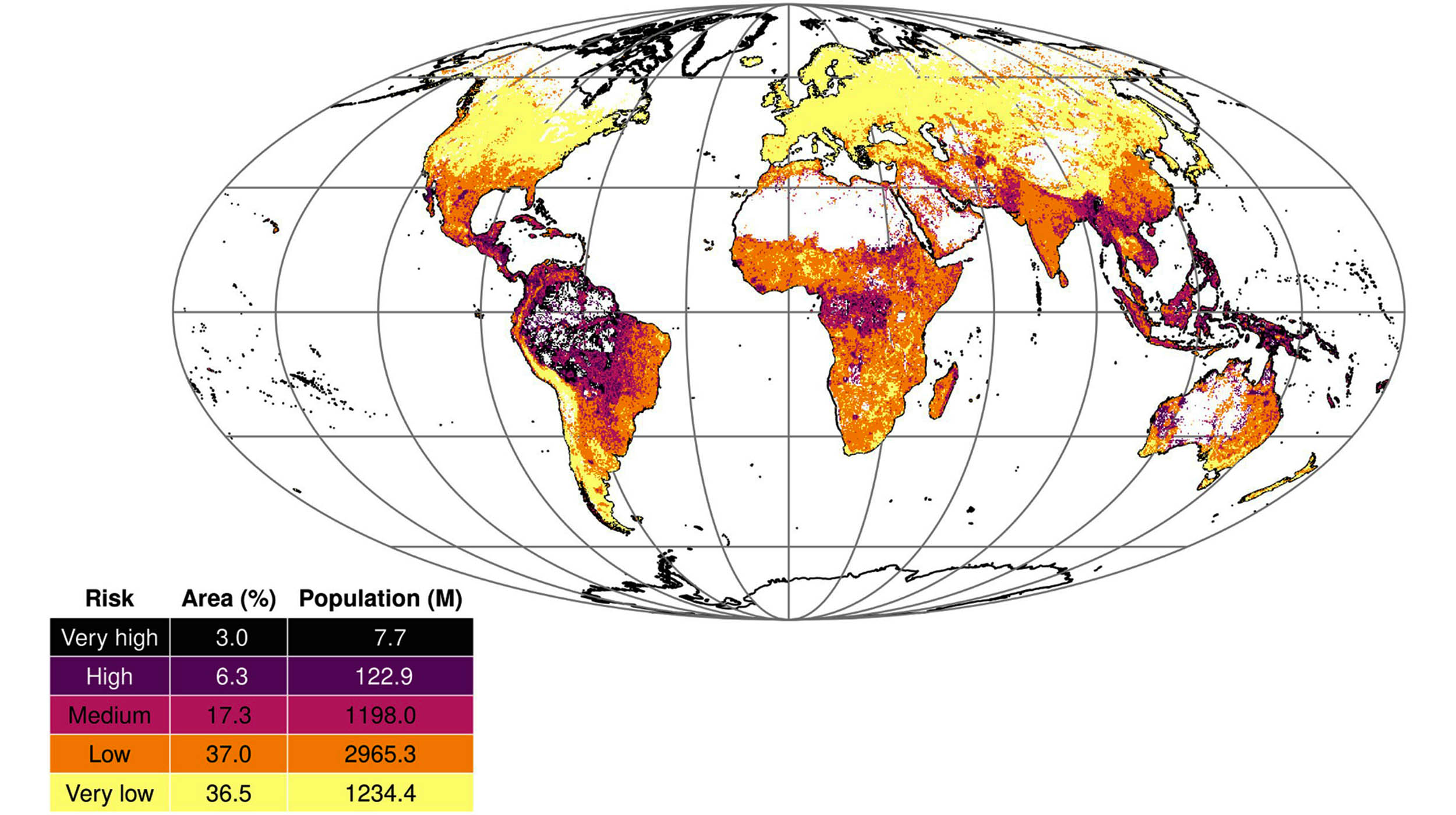
The New Disease Outbreak Map: What Did Scientists Actually Find?
According to the new modeling study (as reported by Earth.com and based on peer‑reviewed research in journals such as Science Advances), researchers combined data on:
- Where new infectious diseases are most likely to emerge
- How quickly they could spread through human populations
- How strong—or fragile—local health systems and surveillance capacities are
Their analysis suggests that roughly one in ten land areas worldwide is highly vulnerable to potentially dangerous outbreaks. These are places where:
- New pathogens are more likely to jump from animals to humans
- Population density or mobility can drive rapid spread
- Health and public health infrastructure may struggle to detect and contain outbreaks early
“Outbreak risk isn’t just about where viruses exist in nature. It’s about where those viruses, people, animals, and weak health systems intersect.”
— Adapted from global health modeling insights published in Science Advances
Why Latin America and Oceania Stand Out as High-Risk Outbreak Hotspots
The map highlights concentrated hotspots across parts of Latin America and Oceania. Several overlapping factors tend to drive outbreak vulnerability in these regions:
- High biodiversity and frequent human–animal contact
Tropical forests and rich ecosystems host thousands of animal species, including bats, rodents, birds, and primates. When people expand agriculture, build roads, or clear forests, opportunities increase for viruses to “spill over” from animals into humans. - Urbanization without matching infrastructure
Fast‑growing cities sometimes outpace clean water, sanitation, and health services, creating fertile ground for diseases like dengue, Zika, and other vector‑borne infections. - Climate sensitivity
Warmer temperatures and changing rainfall patterns can expand the range of mosquitoes and other disease vectors, stretching health systems and surveillance. - Limited health system capacity in some areas
While many countries in these regions have strong medical experts, resources are uneven. Rural and remote communities—especially in parts of Oceania and the Amazon basin—may have limited access to timely diagnostics, treatment, and outbreak investigation teams. - Connectivity and travel patterns
Tourism, trade, and internal migration help economies thrive, but they also speed up how quickly an infection can move between communities and across borders.
These factors don’t doom a region to repeated crises, but they do mean that targeted preparedness—from early warning systems to community health education—is especially important.

How Scientists Measure “Outbreak Vulnerability”
Behind every colorful map is a bundle of data, assumptions, and statistical models. While each research group uses slightly different methods, outbreak vulnerability mapping typically combines three big ideas:
- Hazard – How likely is it that a pathogen will emerge or be introduced?
This can include wildlife diversity, livestock density, previous emergence events, and travel connections from known hotspots. - Exposure – How many people could be exposed, and how quickly?
Factors include population density, local mobility, international travel, and urban vs. rural patterns. - Vulnerability and capacity – How prepared is the system to detect, report, and respond?
Researchers look at health system strength, surveillance capacity, laboratory networks, governance indicators, and sometimes socioeconomic measures like poverty and education.
When these components line up—high hazard, high exposure, and low capacity—you get the “bright red” areas on a disease outbreak risk map.

What This Means for You: Everyday Health, Not Just Headlines
If you live in or travel through a highlighted region, seeing your home on an outbreak map can feel unsettling. It’s important to balance awareness with perspective:
- Outbreak risk is not the same as ongoing danger. Many high‑risk areas go years without major events.
- The same strategies that protect you from “everyday” infections—vaccination, hand hygiene, safe food and water—also reduce your vulnerability in an outbreak.
- Strong communities, informed citizens, and responsive local authorities can dramatically change outcomes when an outbreak does occur.
Personally, some of the most reassuring conversations I’ve had have been with local clinicians in so‑called “hotspot” regions. They often describe quiet, steady work—surveillance, training, drills—that never makes the news but forms the backbone of resilience when alerts go out.

Practical Steps to Protect Yourself in High-Risk Outbreak Regions
Whether you’re a resident, an expat, or a traveler, you can’t control global risk maps—but you can strengthen your own layer of protection. Here are evidence‑informed, realistic steps:
1. Stay Up to Date on Vaccinations
- Follow your country’s routine immunization schedule (e.g., measles, tetanus, influenza).
- If traveling, check WHO or CDC travel health pages for recommended vaccines (e.g., yellow fever, hepatitis A/B, typhoid).
- Consider boosters if it’s been many years since your last dose.
2. Reduce Vector-Borne Disease Risk
- Use EPA‑registered insect repellent on exposed skin.
- Sleep under insecticide‑treated bed nets in areas with malaria or other mosquito‑borne diseases.
- Eliminate standing water around your home or lodging where mosquitoes breed.
3. Practice Smart Hygiene and Food Safety
- Wash hands with soap and water before eating and after bathroom use; carry alcohol‑based hand rub when traveling.
- Prefer freshly cooked, hot foods and safe water sources; be cautious with raw seafood and unpasteurized products where standards are uncertain.
- Use masks and maintain distance in crowded indoor spaces during respiratory outbreaks, when recommended by local health authorities.
4. Prepare for Health Emergencies—Without Panic
- Keep a small “health go‑bag” with essential medications, copies of prescriptions, a thermometer, and basic first‑aid items.
- Know where the nearest clinic, hospital, or telehealth service is—and which languages are spoken.
- Save trusted sources (e.g., WHO, your country’s health ministry, local public health department) for outbreak updates.
Common Challenges: Fear, Misinformation, and “Outbreak Fatigue”
Living through COVID‑19 and other outbreaks has left many people exhausted by health warnings. Seeing yet another map of “danger zones” can trigger:
- Anxiety – Worry that every cough could signal a new pandemic
- Denial – Dismissing all warnings as overblown or political
- Mistrust – Questioning scientific models or public health advice
These reactions are understandable. But they can also make it harder for individuals and communities to respond effectively when a real threat emerges.
How to Navigate These Obstacles
- Use a “two‑source rule.” Before sharing outbreak news, check it against at least two reputable sources (e.g., WHO, major public health agencies, or established news outlets with health reporters).
- Distinguish risk from inevitability. A red area on a map means “pay attention and prepare,” not “panic now.”
- Focus on what you can control. Your vaccines, hygiene, travel choices, and support for local public health measures matter more than the color of the map.
“Preparedness is not about living in fear. It’s about giving ourselves options when the unexpected happens.”
— Public health resilience perspective
How Governments and Health Systems Can Use the New Outbreak Map
While individuals can take important steps, the biggest impact comes when governments and health systems act on vulnerability data. According to global health research and WHO guidance, effective uses of these maps include:
- Targeting investments in laboratories, surveillance networks, and field epidemiology in the highest‑risk districts.
- Strengthening primary healthcare so frontline clinics can recognize unusual patterns earlier.
- Supporting community health workers with training, supplies, and fair pay—especially in rural and remote areas.
- Integrating “One Health” approaches that coordinate human, animal, and environmental health agencies.
- Running realistic simulations and drills to test emergency plans before a real crisis hits.

Before and After Preparedness: How Risk Maps Can Change Outcomes
One helpful way to think about global outbreak maps is to compare what happens in similar regions before and after targeted preparedness. While specifics vary by country, patterns from recent outbreaks are instructive.
Before: Limited Preparedness
- Delayed detection of unusual clusters of illness
- Confusing or absent risk communication
- Overwhelmed hospitals, shortages of basic supplies
- Higher risk of wider spread beyond the initial area
After: Targeted Investments and Planning
- Faster reporting systems and lab confirmation
- Clear guidance to communities and healthcare workers
- Better surge capacity in clinics and hospitals
- Greater chance of containing outbreaks locally
The underlying pathogens may not change—but our ability to cope with them can improve dramatically. That’s the real promise of outbreak vulnerability maps.
Moving From Fear to Informed Action
Seeing nearly 10% of the planet classified as “highly vulnerable” to dangerous disease outbreaks is sobering. It’s also a reminder that global health is deeply interconnected: what happens in Latin American rainforests or remote Pacific islands can ultimately affect us all.
But vulnerability is not destiny. With better surveillance, stronger health systems, transparent communication, and simple protective habits at the individual level, high‑risk regions can become high‑resilience regions.
You don’t need to memorize every hotspot on the map. Instead, you can:
- Keep your vaccinations and basic health checks up to date.
- Follow trustworthy sources for outbreak updates—especially if you live in or travel to highlighted regions.
- Support community and policy initiatives that strengthen public health where you are.
The next time a map like this flashes across your screen, pause, take a breath, and ask: What is one practical step I can take today to be a little more prepared? Then take that step. Preparedness grows one informed decision at a time.
