How a Teen Case of Mono May Echo Years Later—and What You Can Do Now
If you or your teenager has ever battled “the kissing disease”—infectious mononucleosis, or mono—you probably remember the bone-deep fatigue, sore throat, and weeks of feeling like you just couldn’t bounce back. For most people, mono is miserable but temporary.
Emerging research, highlighted in a recent Gizmodo report, suggests that a teenage bout of mono may have a “second act” years later, potentially increasing the risk of certain chronic conditions. That sounds alarming, especially if you or your child has already had mono, but context matters: increased risk does not mean inevitability.
In this article, we’ll unpack what scientists are discovering about mono and long-term health, what symptoms to watch for, and realistic steps you can take now to support your or your teen’s future well-being.
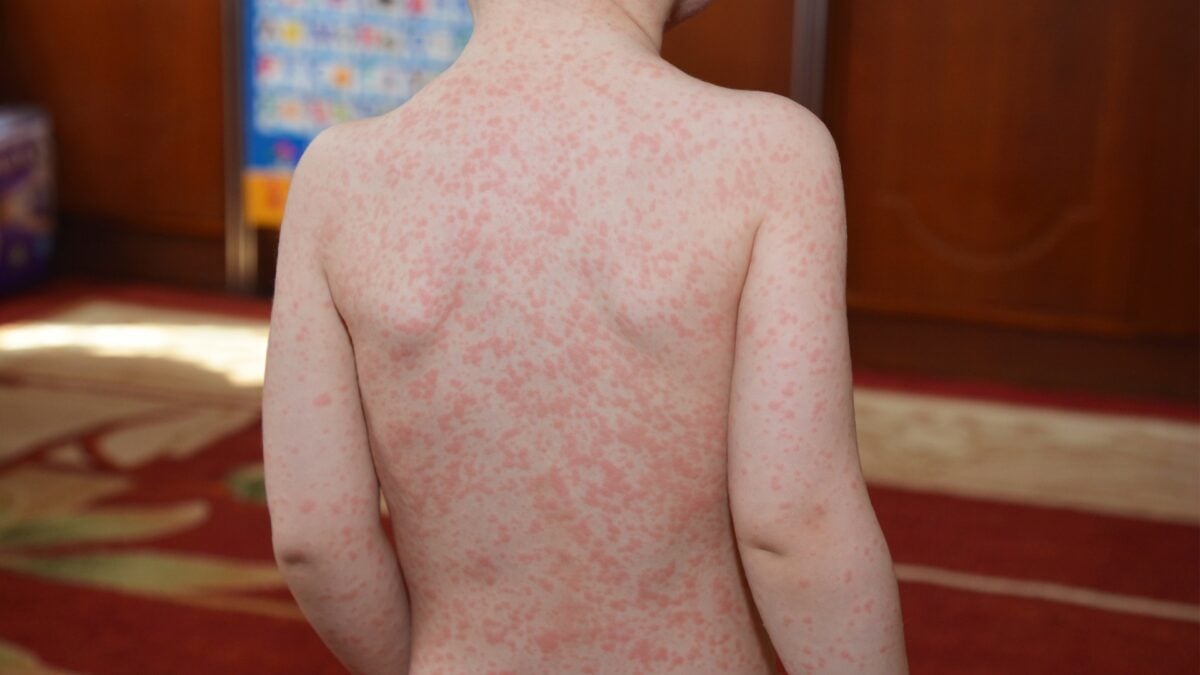
Infectious mononucleosis is usually caused by the Epstein–Barr virus (EBV), a member of the herpesvirus family. EBV quietly infects most people worldwide, often in childhood. When it first strikes during the teen years, it’s more likely to cause full-blown mono: fever, swollen glands, sore throat, and profound fatigue.
The new concern isn’t the acute infection itself, but what might happen long after those symptoms fade. Researchers are investigating whether a history of teenage mono could be one piece of a complex puzzle that leads to certain autoimmune or chronic conditions in a subset of people.
What Exactly Is Mono and Why Is Epstein–Barr Virus So Common?
Infectious mononucleosis is usually triggered by an initial infection with Epstein–Barr virus. EBV is spread mainly through saliva—hence the nickname “kissing disease”—but it can also spread through shared drinks, utensils, or close contact.
- Most people are infected with EBV at some point in their lives.
- If infection happens in early childhood, symptoms can be mild or absent.
- In teens and young adults, first-time infection more often leads to classic mono.
Typical mono symptoms include:
- Severe fatigue
- Sore throat
- Swollen lymph nodes in the neck
- Fever and chills
- Enlarged spleen or liver (in some cases)
After the acute phase, EBV doesn’t disappear. Like other herpesviruses, it stays in the body in a latent, or “quiet,” state, usually controlled by the immune system. The new research is exploring how that lingering virus may, in some people, interact with genetics and environmental factors to influence disease risk years later.
What New Research Suggests About Teenage Mono and Long-Term Health
The study discussed in the Gizmodo article adds to a growing body of evidence linking past EBV infection—especially when it caused symptomatic mono—with a higher risk of certain chronic conditions later in life. While details vary by study, researchers are most concerned about:
- Autoimmune diseases, such as multiple sclerosis (MS) and some types of lupus
- Certain chronic fatigue–like syndromes in a subset of people after severe viral illness
- Very rare EBV-associated cancers, such as some lymphomas and nasopharyngeal carcinoma
“Epstein–Barr virus is one of the most successful human viruses. It infects most of us and typically coexists quietly. But in genetically susceptible individuals, especially after symptomatic mono, it may act as a trigger that nudges the immune system off course.”
— Immunology researcher, commentary on EBV and autoimmune risk
Importantly, an increased relative risk does not mean that most people who had mono will develop these conditions. For example, some large cohort studies have shown a strong association between prior EBV infection and multiple sclerosis, yet MS remains a relatively rare disease overall.
Think of mono as one potential “spark” in a pile of wood: genetics, other infections, environmental exposures, and lifestyle factors all shape whether that spark fades out or contributes to a fire. The presence of the spark alone doesn’t guarantee a blaze.
How Could a Teen Infection Cause Problems Years Later?
Scientists are still piecing together the mechanisms, but several plausible pathways have emerged from laboratory and population studies:
- Molecular mimicry. Some EBV proteins resemble human proteins. When the immune system attacks the virus, it may occasionally “cross-react” with the body’s own tissues in susceptible individuals, contributing to autoimmunity.
- Long-term B-cell changes. EBV lives primarily in B cells (a type of white blood cell). Persistent infection might subtly alter how these cells behave, influencing immune responses over time.
- Immune system “reprogramming.” Severe viral illness during a critical developmental window (like adolescence) may reshape immune signaling pathways, affecting how the body responds to later triggers.
- Chronic low-level inflammation. In some people, residual immune activation after infection might maintain a slightly “revved up” state, which in turn can raise the odds of certain chronic diseases.
These are active areas of research rather than settled facts. What’s clear is that EBV is more than a short-lived nuisance; it’s a long-term guest in our immune system, and scientists are finally learning how that long-term relationship may shape health.
A Real-World Story: From “Just Mono” to Staying Proactive
Consider a composite example that reflects what many families experience:
At 16, Alex came down with mono mid–school year. For nearly two months, they struggled with overwhelming fatigue, a painful sore throat, and missed classes. Doctors recommended rest, no contact sports (to protect an enlarged spleen), and regular check-ins. By summer, Alex felt mostly like themself again and resumed normal activities.
Fast-forward eight years. Now in their mid-20s, Alex starts noticing persistent fatigue, brain fog, and odd neurological sensations. Because Alex remembered that mono can sometimes have longer-term implications, they brought it up with their primary care clinician early. That conversation led to timely referrals, lab work, and a neurologist’s evaluation that ruled out some serious conditions and identified others that could be managed with lifestyle changes and treatment.
Not everyone who has mono will follow Alex’s path—many people never experience lingering issues. But Alex’s story illustrates why awareness matters: not to spark anxiety, but to encourage earlier, informed care if something doesn’t feel right.
After Mono: Symptoms You Shouldn’t Ignore
Most people recover from mono within several weeks to a few months. Still, it’s wise to stay attuned to changes in your body in the years that follow, especially if you had a severe case during the teen years.
Talk with a healthcare professional if you notice:
- Fatigue that lasts for more than a few months and significantly limits daily activities
- New or worsening neurological symptoms, such as changes in vision, numbness, balance problems, or muscle weakness
- Unexplained weight loss, night sweats, or persistent fevers
- Swollen lymph nodes that don’t go away or keep getting larger
- Ongoing pain, particularly if associated with joint swelling or a rash
None of these signs automatically mean that mono “caused” a problem, but your history can help clinicians interpret them and decide what evaluations are necessary.
Practical, Evidence-Informed Steps to Support Long-Term Health After Mono
There’s currently no way to “erase” EBV from the body, and no guaranteed method to prevent all potential long-term effects. However, several strategies are grounded in good immune health and early detection principles.
1. Document your history
- Keep a record of the approximate date you had mono and how severe it was.
- Share this history with new healthcare providers, especially if you develop unexplained symptoms later.
2. Respect recovery time
Pushing through the fatigue too aggressively during recovery can prolong symptoms.
- Gradually resume activity rather than jumping back into intense sports or late nights.
- Work with schools or employers on temporary accommodations.
3. Support general immune and brain health
While no lifestyle change can guarantee protection, the same habits that reduce overall chronic disease risk are likely helpful here:
- A balanced diet rich in plants, fiber, and healthy fats
- Regular physical activity appropriate to your energy level
- Consistent, good-quality sleep
- Stress-management practices, such as mindfulness or counseling
- Not smoking or vaping, and limiting alcohol
4. Stay updated on vaccines and research
Pharmaceutical companies and academic groups are actively working on EBV vaccines, some of which are in early clinical trials. While these are not yet available for general use, they signal a growing recognition of EBV’s role in chronic disease.
Periodically checking reputable sources such as the U.S. Centers for Disease Control and Prevention (CDC) or the World Health Organization (WHO) can keep you informed as evidence evolves.
A Visual Look at Mono and Long-Term Risks


If You Had Mono as a Teen, How Worried Should You Be?
It’s understandable to feel uneasy reading about mono’s possible “second act.” Many adults only now realize their teenage illness might be relevant to today’s health. A few clarifying points may help:
- Risk is increased, not absolute. Even in studies showing strong associations, the majority of people with past mono do not go on to develop serious chronic conditions.
- You can’t change the past infection. Worrying about something that already happened is draining. Focus on what you can influence now: lifestyle, early symptom recognition, and regular preventive care.
- Your history is one data point. Clinicians consider many factors—family history, current symptoms, exam findings, and tests—not just a past mono diagnosis.
“Knowing you had mono in high school doesn’t mean you’re destined for chronic illness. It simply gives you and your healthcare team another piece of information to guide wise, proactive care.”
— Primary care physician, adolescent medicine
For Parents and Caregivers: Supporting a Teen Through Mono and Beyond
Watching a teenager struggle with weeks of exhaustion and missed activities is hard. Add headlines about long-term risks, and it’s easy to feel overwhelmed.
Some practical ways to help:
- Validate their fatigue and symptoms rather than brushing it off as “just being tired.”
- Coordinate with schools or coaches to reduce demands during recovery.
- Model balanced health behaviors—regular meals, bedtime routines, and screen-time limits.
- Encourage open communication about any new or worrying symptoms in the months and years ahead.
Trusted Resources to Stay Informed
For up-to-date, evidence-based information on mono, Epstein–Barr virus, and related conditions, consider:
- U.S. Centers for Disease Control and Prevention (CDC): Epstein–Barr Virus and Infectious Mononucleosis
- National Institute of Neurological Disorders and Stroke: Multiple Sclerosis
- World Health Organization: Epstein–Barr Virus (EBV) overview
- Peer-reviewed journals accessible through platforms like PubMed for the latest EBV and autoimmunity research.
When reading about health online, prioritize sources that cite scientific studies, acknowledge uncertainty, and avoid miracle cures or fear-based messaging.
Looking Ahead: From Fear to Informed Action
A teenage bout of mono is more than an unpleasant memory; it’s part of your health story. The latest research suggests it may influence long-term risk for certain conditions, but it’s only one factor among many, and it does not doom you to chronic illness.
The most constructive path forward is to stay informed, take good care of your overall health, and seek medical guidance early if something feels off. Keeping an honest, ongoing dialogue with a trusted healthcare professional is far more powerful than worrying alone.
If you or your teen has a history of mono, consider taking these steps this week:
- Write down your mono history (approximate dates, severity) and store it with your medical records.
- Schedule a routine checkup if you haven’t had one in the past year.
- Choose one sustainable habit—better sleep, a short daily walk, or a more balanced meal—to support long-term health.
You can’t change that past infection, but you can absolutely influence what comes next.
