The Teen Whose Pain Wasn’t “All in Her Head”: How One MRI Finally Revealed a Hidden Condition
For months, 17-year-old Spring teen Myra Fennell battled severe, unexplained pain that some doctors dismissed as being “all in her head,” until a Memorial Hermann physician looked closer at her MRI and uncovered a rare condition that had been overlooked. Her story reveals how easily complex pain can be misunderstood, and how persistence, careful imaging, and listening to patients can finally bring answers and relief.

When Pain Is Dismissed — Until One MRI Changes Everything
If you’ve ever been told your pain is exaggerated, stress-related, or simply “in your head,” Myra’s story will feel painfully familiar. What began as a healthy, active teen’s life in Spring, Texas, turned into an exhausting circuit of appointments, questions, and doubt when her body suddenly stopped cooperating — and no one could explain why.
It wasn’t until a Memorial Hermann specialist took a fresh look at her MRI that the real problem came into focus: a rare medical condition that had been hiding in plain sight on earlier scans. That moment didn’t instantly erase her pain, but it gave her something every patient deserves — an explanation and a path forward.
“What hurt the most wasn’t just the pain itself,” Myra later reflected, “it was feeling like nobody believed me. That all changed when one doctor finally said, ‘I see it.’”
A Teen’s Life Interrupted: How Myra’s Pain Began
Before her symptoms started, Myra was a typical Spring High School junior — juggling classes, friends, and extracurriculars. Then came a sharp, relentless pain that seemed to spread and intensify over weeks. Simple routines became battles: getting out of bed, walking down the hallway, sitting through class.
Like many families do, her parents sought answers through their local doctors. Myra underwent:
- Basic blood tests to look for infection or inflammation
- Initial imaging scans that were read as “unremarkable”
- Trial medications for pain and muscle relaxation
Yet the pain didn’t match the reassuring test results. When nothing obvious appeared on early scans and lab work, some clinicians began asking if stress, anxiety, or mood might be the “real” problem. That line of questioning is common — but for Myra, it felt like a quiet accusation.
One doctor reportedly told the family that adolescents “often somaticize stress,” suggesting that her pain might be more psychological than physical.
“All in Your Head”: The Hidden Cost of Medical Dismissal
Being told your pain is “all in your head” can be devastating — especially for a teenager still figuring out who she is. For Myra, each appointment that ended with a shrug or a suggestion of anxiety chipped away at her confidence.
Evidence from pain research backs up what she felt:
- Chronic pain is complex — involving the nervous system, immune system, and often mood — but that complexity doesn’t mean pain isn’t real.
- Teen patients with unexplained pain often see multiple providers before receiving a diagnosis, increasing stress and health-care costs.
- Early dismissal can delay treatment, potentially allowing underlying conditions to worsen.
Myra’s family, however, wasn’t ready to give up. They sought a second opinion through the Memorial Hermann system — a step that would change everything.

The MRI That Finally Revealed a Rare Condition
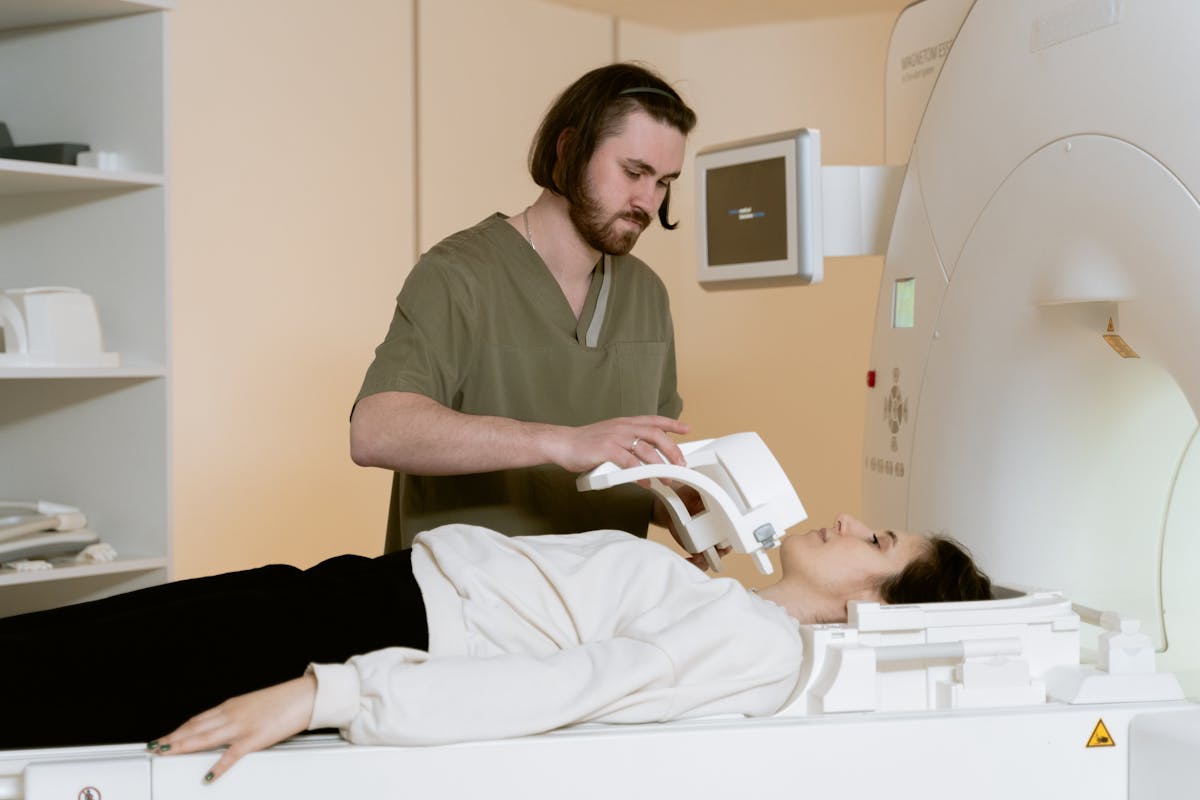
At Memorial Hermann, Myra underwent a more detailed evaluation. A specialist reviewed her history and pain pattern, then ordered targeted imaging — including a new MRI study. On the surface, it looked similar to her previous scans. But this time, a radiologist and physician took a closer, more focused look.
Somewhere in the grayscale swirls of bone, nerves, and soft tissue, they saw it: subtle but significant changes consistent with a rare medical condition that had been overlooked. While the Houston Chronicle report highlights the privacy of Myra’s exact diagnosis, clinicians familiar with such cases point to possibilities such as:
- Unusual structural issues in the spine or joints
- Rare nerve entrapment or compression syndromes
- Less common inflammatory or vascular disorders
“The findings were subtle,” one Memorial Hermann doctor noted, “but once you know to look for them, they tell a clear story. The MRI finally matched what Myra had been describing all along.”
For Myra and her family, the discovery was a turning point — not a magical cure, but validation. There was a name, an explanation, a reason the pain had been so intense.
From Diagnosis to Daily Progress: Myra’s Rehabilitation Journey
With the diagnosis in hand, Myra’s team could finally build a tailored plan. For her, that meant a combination of medical management and specialized physical therapy at Spring Physical Therapy — the clinic where the Houston Chronicle photographed her in March 2026.
Under the guidance of therapists experienced with complex pain and rare conditions, Myra worked through:
- Gentle mobility exercises to restore movement without aggravating her symptoms.
- Targeted strengthening of muscles that support the affected joints and structures.
- Pain education — understanding how nerves, brain, and body process pain signals.
- Gradual exposure back to activities she loved, pacing carefully to avoid flares.

Progress wasn’t linear. Some weeks, Myra felt almost like herself again. Other weeks, a flare would send her back to the couch. Her treatment team emphasized that this up-and-down pattern is normal in complex pain recovery, and that long-term improvement matters more than any single day’s symptoms.
What Myra’s Story Teaches Us About Listening to Pain
Myra’s experience isn’t an isolated story — it’s a lens into how modern medicine handles rare conditions and chronic pain, especially in young people. While every case is unique, her journey highlights several evidence-informed lessons:
- Patients are experts in their own experience. Even when tests are inconclusive, a consistent story of severe, function-limiting pain deserves respect and careful evaluation.
- Rare conditions are easy to miss. By definition, most clinicians see them rarely. Second opinions and subspecialty care can make the difference.
- Imaging must be interpreted in context. Subtle MRI findings can be significant when they line up with symptoms; “incidental” findings can also be misleading if taken out of context.
- Validation is therapeutic. Studies show that feeling believed and supported can reduce anxiety, improve treatment engagement, and even lessen perceived pain intensity.
“We tell every trainee the same thing,” said one Memorial Hermann specialist. “Diagnose with humility. If the picture doesn’t fit, don’t force it — look again.”
If You’re in Unexplained Pain: Practical Steps to Advocate for Yourself
You may not have access to the exact specialist who helped Myra, but you can borrow some of the strategies that ultimately led to her diagnosis. These steps aren’t a guarantee of answers, yet they can improve your chances of being heard and receiving appropriate care.
- Track your symptoms clearly.
Keep a simple log for 1–2 weeks:- Where the pain is
- What it feels like (sharp, dull, burning)
- What makes it better or worse
- How it affects your daily activities
- Bring a supporter.
A parent, partner, or friend can:- Help you remember details during appointments
- Confirm how your pain affects your life
- Provide emotional backing if you feel dismissed
- Ask focused questions.
For example:- “What conditions are you ruling out with these tests?”
- “If the tests are normal but my pain continues, what’s the next step?”
- “Would a specialist or second opinion be appropriate?”
- Consider a second opinion — respectfully.
Second opinions are standard in complex care. They’re not accusations; they’re about safety and thoroughness. - Address mental health without accepting blame.
Counseling, stress management, and coping strategies can help you live better with pain — even while you and your doctors continue searching for physical causes.

Common Obstacles on the Way to a Diagnosis (and How to Navigate Them)
Myra’s path from first symptoms to diagnosis wasn’t straightforward — and most people with rare or complex conditions face similar hurdles. Recognizing these patterns can help you prepare for them.
- Obstacle: “Normal” tests with abnormal pain.
Response: Ask whether further imaging, different types of scans, or repeat studies over time might be helpful. - Obstacle: Limited appointment time.
Response: Bring a written summary of your key concerns so you can focus on the most important points quickly. - Obstacle: Feeling intimidated.
Response: It’s okay to say, “I’m having trouble understanding this. Could you explain it in another way?” Clear communication is part of good care. - Obstacle: Insurance or referral barriers.
Response: Ask your primary clinician, “How can we document medical necessity for a specialist or advanced imaging?” Social workers or patient navigators can sometimes help.

You’re Not Invisible: Finding Hope in Stories Like Myra’s
Myra Fennell’s journey from a dismissed “mystery pain” to a clearly defined, rare diagnosis at Memorial Hermann doesn’t promise that every person with chronic pain will find easy answers. But it does show what’s possible when patients refuse to be brushed aside, families persist, and clinicians keep looking until the story finally makes sense.
If you’re living with unexplained pain, know this:
- Your pain experience is real, whether or not you have a diagnosis yet.
- It’s reasonable — not rude — to ask for clearer explanations and second opinions.
- Progress may be slow and uneven, but small gains still matter.
You deserve to be heard, believed, and cared for with curiosity rather than dismissal. Myra’s story is one of many — and while every medical journey is different, yours is worth pursuing with the same determination.
Call to action: If you or someone you love is facing persistent, unexplained pain, consider scheduling a dedicated visit with your clinician to review the full story — not just the latest test result — and, if needed, ask what it would take to get a second opinion or specialized imaging review.
Where to Learn More About Chronic and Complex Pain
For deeper, evidence-based information on chronic pain, rare conditions, and patient advocacy, explore:
- CDC – Chronic Pain: Overviews on chronic pain, prevalence, and treatment approaches.
- National Institute of Neurological Disorders and Stroke – Pain Information: Science-based explanations of different pain conditions.
- NIH Genetic and Rare Diseases (GARD) Information Center: Reliable information about rare conditions and support resources.
- World Health Organization – Pain Management: Global perspectives on access to pain care.
