New TB Tests at the Frontlines: How WHO’s Latest Guidance Can Help End Tuberculosis
On World TB Day, the World Health Organization (WHO) called on countries to accelerate efforts to end tuberculosis by rolling out new, faster diagnostic tools that can be used closer to where people live and seek care. If you work in public health, run a clinic, or simply care about TB in your community, you may be wondering what these new tests are, whether they really work, and how to realistically integrate them into often overstretched health systems.
This guide walks you through WHO’s latest recommendations on TB diagnostics, what the evidence says, and practical steps to expand access—without overpromising, and with full acknowledgment of the very real constraints many countries face.
The TB Diagnosis Gap: Why WHO Is Pushing New Tests Now
Despite being preventable and curable, tuberculosis remains one of the top infectious disease killers worldwide. WHO estimates that millions of people with TB are “missed” each year—either never diagnosed or diagnosed too late for effective treatment or infection control.
- Many people with TB live far from laboratories with advanced equipment.
- Classic smear microscopy can miss a large share of cases, especially among people living with HIV or children.
- Delays in sending samples to centralized labs mean delays in starting treatment and in detecting drug resistance.
In its latest technical update around World TB Day, WHO emphasized expanding access to near point-of-care molecular tests and other innovative tools that bring accurate diagnosis closer to patients. The goal is not just better technology, but faster, more equitable detection of TB and drug-resistant TB.
“Ending TB is impossible if people are never diagnosed. New diagnostic tools are only as powerful as our ability to deploy them at the primary care and community level.” — Global TB Programme advisor, summarizing WHO’s latest guidance
What’s New in WHO’s TB Diagnostic Recommendations?
WHO’s recent updates build on existing guidance but push harder toward decentralization and rapid molecular testing. While details evolve as evidence accumulates, several themes stand out in the latest communications and guideline updates up to early 2026:
- Near point-of-care molecular tests as an initial diagnostic test
Molecular assays (for example, cartridge-based or portable PCR-like systems) are increasingly recommended as the first test for people with presumptive TB, especially in high-burden settings, because they:- Detect TB more accurately than smear microscopy.
- Can rapidly identify resistance to key drugs like rifampicin.
- Produce results in hours rather than days or weeks.
- Decentralization to primary-care and community settings
WHO is encouraging placement of certain molecular platforms in:- District hospitals and busy primary care clinics.
- Mobile units serving remote communities.
- HIV, diabetes, and antenatal clinics where people at higher risk already seek care.
- Diverse sample types
For people who cannot easily produce sputum (for example, children, some people living with HIV), WHO highlights accumulating evidence for:- Stool samples for pediatric TB in specific contexts.
- Non-sputum respiratory samples (like nasopharyngeal aspirates) where feasible.
- Improved tests for drug resistance
Rapid molecular tests can screen for resistance to isoniazid, fluoroquinolones, and other second-line drugs in addition to rifampicin, helping clinicians move faster to effective regimens.
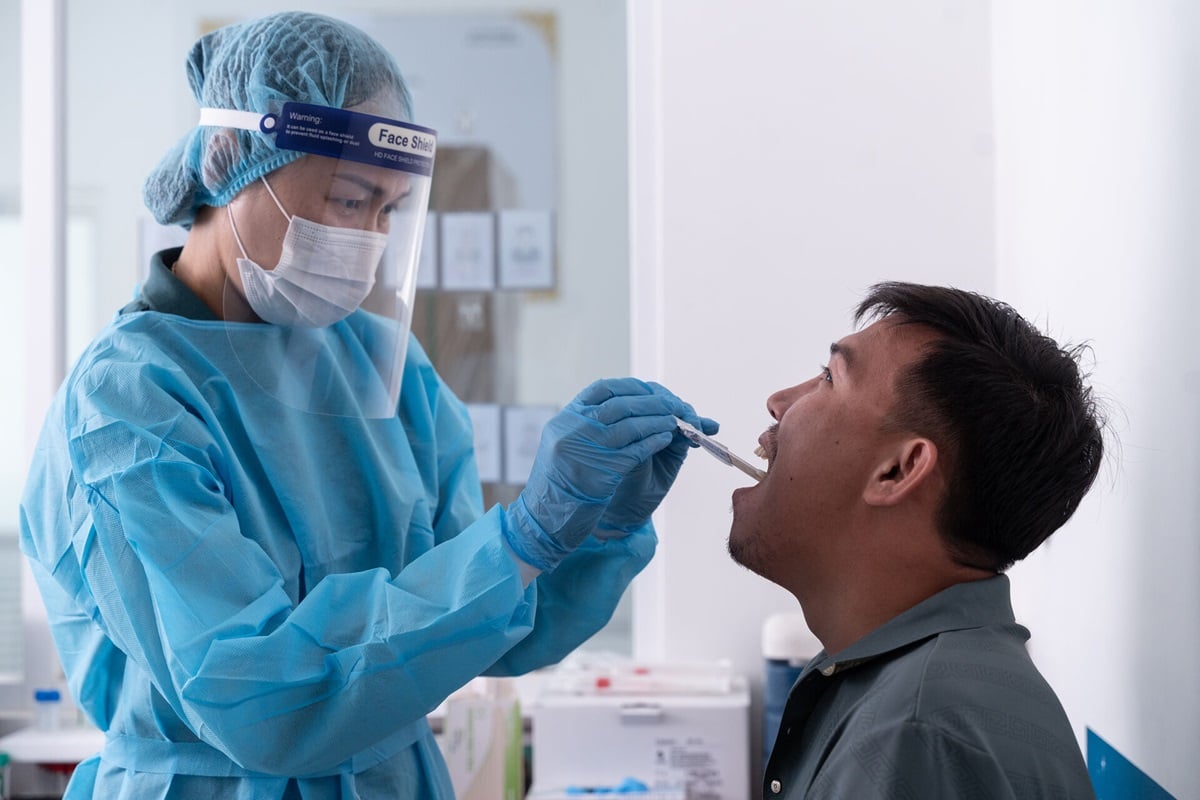
The Science Behind New TB Tests: What the Evidence Shows
WHO recommendations are based on systematic reviews, meta-analyses, and field evaluations rather than individual studies alone. While individual test brands differ, several robust trends have emerged.
- Higher sensitivity than smear microscopy
Molecular assays typically detect more TB cases, particularly among:- People living with HIV.
- Children.
- People with paucibacillary or extrapulmonary disease.
- Rapid turnaround for drug resistance
Many WHO-recommended molecular tests can detect rifampicin resistance within hours, a crucial proxy for multidrug-resistant TB (MDR-TB) in many settings. - Operational performance in the field
Implementation studies show that when machines are well maintained and supply chains are stable, molecular testing:- Shortens the time to treatment initiation.
- Improves linkage to appropriate MDR-TB care.
- Reduces loss to follow-up between testing and treatment.
However, these gains are not automatic. Benefits are blunted when cartridges stock out, power is unreliable, or results fail to reach clinicians and patients promptly. WHO repeatedly emphasizes that new diagnostics must be embedded in strong systems, not simply dropped into existing gaps.
What “Near Point-of-Care” TB Testing Really Looks Like
“Point-of-care” can sound abstract. In practice, WHO often talks about near point-of-care—placing relatively simple molecular platforms in facilities that are closer to patients than central reference labs, but still have minimal infrastructure.
Typical near point-of-care TB testing sites include:
- District hospitals with basic lab rooms.
- Larger primary health centers serving high TB burden areas.
- Integrated TB/HIV clinics.
- Mobile clinics visiting mining communities, informal settlements, or remote villages.
These sites may not have advanced biosafety cabinets or highly specialized technologists. Instead, WHO-recommended near-POC platforms are generally:
- Cartridge-based, reducing hands-on processing.
- Automated, with built-in controls.
- Designed to run on simple power sources, sometimes with battery backup.

Turning WHO Guidance into Action: A Step-by-Step Implementation Plan
Rolling out new TB diagnostics is a journey, not a single procurement. Below is a practical framework you can adapt at national, provincial, or large facility level.
- Map your diagnostic landscape
- Where are existing TB microscopy and molecular testing sites?
- Where do most people with TB symptoms first seek care?
- Where are the biggest gaps in access or turnaround time?
- Prioritize high-impact locations
- High-burden districts with long travel distances to a central lab.
- Facilities serving populations with high HIV prevalence, miners, prisoners, or urban poor communities.
- Sites with stable power and staffing where additional support is realistic.
- Choose WHO-recommended platforms aligned with your context
- Check each platform’s WHO policy status and indication (initial test vs. add-on; drug resistance coverage).
- Consider cartridge cost, warranty, local service availability, and data connectivity options.
- Avoid relying on a single supplier where possible to reduce vulnerability to stockouts.
- Strengthen sample referral and result return systems
- Design simple sample transport routes for facilities without machines.
- Use SMS, secure messaging apps, or electronic medical records to send results back quickly.
- Establish SOPs so clinicians know how to act on molecular and drug-resistance results.
- Train and support staff
- Include both lab personnel and clinicians in training, emphasizing clinical decision-making, not just machine operation.
- Provide job aids, refresher trainings, and remote mentoring where possible.
- Monitor performance and equity
- Track key indicators: test volumes, positivity rates, error rates, time from test to treatment.
- Disaggregate by sex, age, region, and risk group to detect inequities.
- Use data to adjust placement of machines and resources over time.
A Real-World Story: From Three Visits to One
In a rural district hospital (fictionalized, but based on patterns seen in several countries), patients with chronic cough used to make up to three trips before getting a confirmed TB diagnosis:
- First visit: symptom evaluation, sputum smear sent to a distant lab.
- Second visit (days later): smear-negative result; no further testing due to distance and cost.
- Third visit: patient returns even sicker; TB finally suspected again and sample re-sent.
After the hospital introduced a WHO-recommended molecular platform:
- Most patients with TB symptoms gave a sample on the same day as their first visit.
- Results were available within a few hours.
- Clinicians could start treatment for many patients on the same or next day.
- Some patients with rifampicin resistance were identified early and referred for appropriate MDR-TB care.
Not every patient was reached; some still faced transport costs or stigma. But the shift from multi-visit, uncertain diagnosis to faster, more reliable testing reduced loss to follow-up and provided tangible proof that WHO’s recommendations can be translated into better patient journeys when systems support them.
Common Barriers to New TB Diagnostics—and How to Overcome Them
Many programs are convinced by the science, but struggle with practical barriers. WHO’s technical support and country experiences suggest several strategies.
1. Cost and Financing
Molecular tests cost more per test than smear microscopy, especially when factoring in machine purchase, cartridges, and maintenance.
- Leverage global mechanisms such as the Global Fund, Unitaid, or pooled procurement systems.
- Use cost-effectiveness and budget impact analyses to advocate for domestic funding.
- Target high-yield sites first instead of spreading machines too thinly.
2. Human Resources and Training
Staff turnover, limited lab expertise, and competing priorities can undermine implementation.
- Develop simple, visual SOPs and quick-reference guides.
- Pair new sites with mentor labs or regional supervisors.
- Integrate TB diagnostic training with broader lab strengthening initiatives.
3. Infrastructure and Maintenance
Power cuts, equipment breakdowns, and delayed repairs can halt testing.
- Assess power stability, temperature, and space before site selection.
- Negotiate service contracts and preventive maintenance schedules with suppliers.
- Keep basic spare parts and backup power options where possible.
4. Data and Quality Assurance
Without data, it’s hard to know whether new diagnostics are working as intended.
- Integrate machines with digital tools that automatically capture and transmit results where possible.
- Participate in external quality assessment (EQA) and proficiency testing schemes.
- Regularly review error logs and invalid test rates to flag training or maintenance needs.
What This Means for People at Risk of TB
If you are a patient, caregiver, or community advocate, you may not be choosing diagnostic platforms—but WHO’s recommendations can still empower you to ask for better care.
- If you have a persistent cough (2 weeks or more), fever, night sweats, or weight loss, ask if TB testing is available.
- In many high-burden settings, molecular testing is now recommended as the first test for suspected TB—ask what tests are used and when.
- If you are living with HIV, pregnant, or have diabetes, mention this to your provider; it may influence testing decisions.
- Do not delay returning for results or starting treatment if TB is confirmed; early treatment improves outcomes and reduces transmission.
Before and After: How New TB Diagnostics Change the Care Pathway
The impact of WHO-recommended diagnostics becomes clearer when we compare the typical patient journey before and after implementation.

While these images represent ideal scenarios, they capture a crucial point: WHO’s diagnostic recommendations are ultimately about people spending less time in uncertainty and more time receiving effective care.
Insights from WHO and Global TB Experts
WHO collaborates with researchers, national TB programs, civil-society groups, and funders to continuously refine its guidance. Several recurring messages emerge from these expert dialogues:
“Diagnostics are not a luxury. They are the foundation of any serious TB elimination strategy. Every undiagnosed person is a missed opportunity to save a life and prevent transmission.”
“New tools alone will not end TB. But without them, we will continue to rely on outdated methods that leave the most vulnerable behind.”
These perspectives align with WHO’s broader strategy: pairing innovative tools—diagnostics, shorter treatment regimens, preventive therapy—with strong health systems, political commitment, and community engagement.
Key Takeaways and Next Steps for Ending TB
WHO’s renewed call on World TB Day is clear: to end TB, countries must close the diagnostic gap. New, near point-of-care TB tests are powerful tools to help do that—but only if they are planned, financed, and implemented thoughtfully.
- New WHO-recommended molecular tests detect more TB, faster, and closer to where people live.
- Decentralization to primary care and community settings is essential for equity.
- Successful implementation depends on financing, training, maintenance, and strong data systems.
- Patients and communities can play an active role by seeking testing and advocating for quality care.
Whether you are a policymaker, program manager, clinician, or advocate, your next step could be as concrete as reviewing your country’s diagnostic algorithm against WHO’s latest guidance, joining a working group on TB diagnosis, or simply ensuring that every person with TB symptoms in your facility is offered testing.
Ending TB is ambitious—but each timely, accurate diagnosis is a step toward that goal. The tools are here; the challenge now is to use them where they are needed most.
What You Can Do Today
Depending on your role, consider taking one of these actions in the next week:
- Health officials: Convene a brief meeting to review current TB testing coverage and identify priority sites for near-POC expansion.
- Clinicians: Check your facility’s TB diagnostic algorithm and ensure it reflects the latest WHO guidance where feasible.
- Laboratory managers: Audit your existing TB platforms, error rates, and stock levels; flag systemic issues early.
- Community advocates: Share accurate information on TB symptoms and the importance of early testing through local networks.
Change rarely happens overnight, but incremental, evidence-based improvements—like adopting better TB diagnostics—can save lives quietly, day after day. That is the real power behind WHO’s call to action this World TB Day.
