How Routine Mammograms Could Quietly Save Your Heart, Too
Routine breast cancer screenings may also offer an unexpected window into your heart health.
For many women, the annual mammogram is a familiar, if not exactly welcome, part of staying on top of breast cancer risk. What’s less known is that those very same images may hold vital clues about the risk of heart disease—the leading cause of death in women, often striking silently for years.
A new study published in the European Heart Journal and covered by The Washington Post reports that artificial intelligence (AI) can analyze routine mammograms to detect signs of calcium build-up in arteries—an important red flag for future heart disease. This doesn’t replace traditional heart screening, but it may give many women an earlier, easier opportunity to understand their cardiovascular risk.
In this guide, we’ll explore how mammograms can reveal heart disease risk, what this new AI technology actually does, and how you can use this information to advocate for your own health in a calm, informed way—without panic, over-testing, or false promises.

Why Heart Disease in Women Is So Often Missed
Heart disease is responsible for roughly one in three deaths in women worldwide, yet it often receives less attention than breast cancer. Part of the problem is that women’s heart symptoms can be subtle, easily dismissed, or attributed to stress, fatigue, or aging.
- Risk builds quietly over years through blood pressure, cholesterol, and lifestyle factors.
- Women are sometimes less likely to be referred for cardiac testing, especially if they’re younger or don’t have “classic” chest pain.
- Many women are diligent about breast screenings but may rarely get a targeted heart evaluation before problems appear.
This is where the new research becomes so compelling: it suggests that a test many women are already getting—the mammogram—could double as an early warning system for their hearts.
How AI Finds Heart Risk on a Mammogram
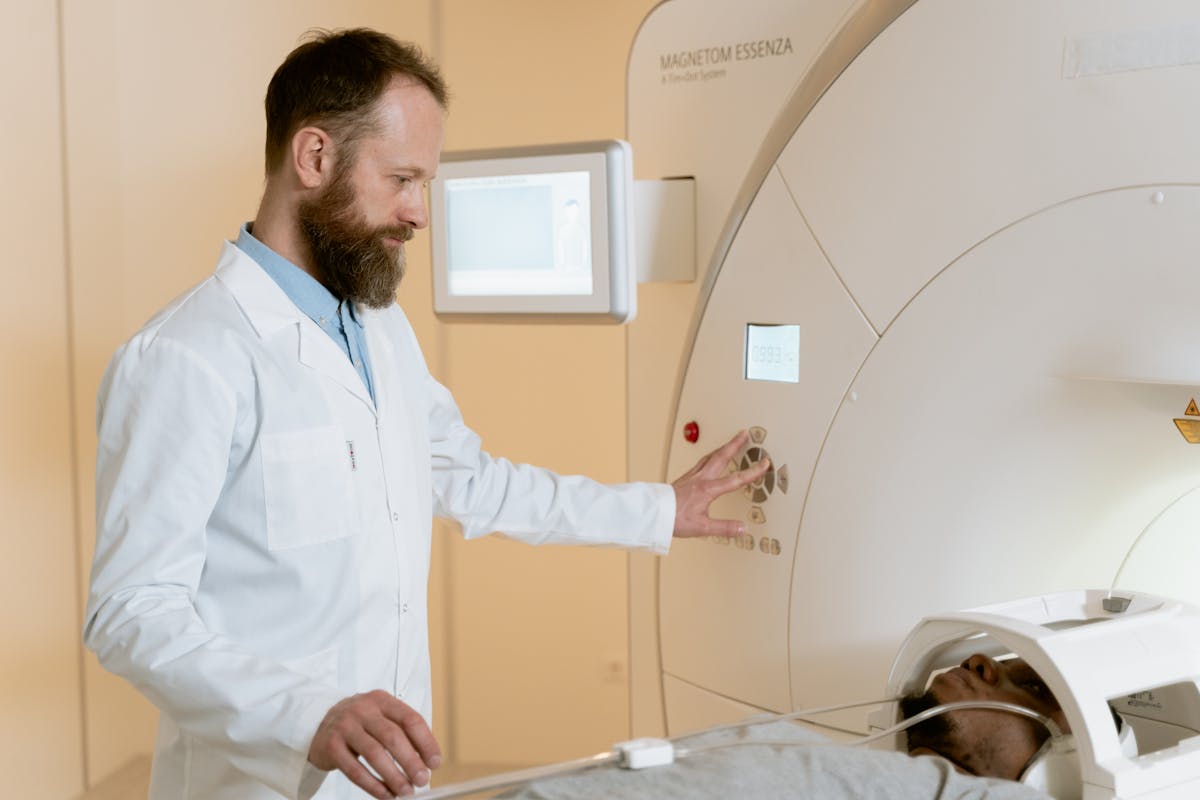
A mammogram is an X-ray image of the breast. Traditionally, radiologists read these images to look for signs of breast cancer—like masses, architectural distortions, or tiny calcium deposits (microcalcifications) in breast tissue.
The new AI tools described in the European Heart Journal study do something different: they scan the same images for calcium deposits in the arteries—especially in the vessels that supply the breasts and chest wall. This is called breast arterial calcification (BAC), and it can be a marker of underlying cardiovascular disease.
- The AI is trained on thousands of mammograms linked to known cardiovascular outcomes.
- It “learns” to distinguish normal tissue from arterial calcium patterns.
- It generates a score or classification indicating how much arterial calcification is present.
- That information can then be combined with traditional risk factors (age, blood pressure, cholesterol, smoking, etc.).
In the study covered by The Washington Post, women whose mammograms showed higher levels of arterial calcification had a significantly increased risk of future cardiovascular events, even when they had no symptoms at the time.
“Breast arterial calcification on routine mammography is emerging as a powerful marker of cardiovascular risk in women. It doesn’t diagnose heart disease by itself, but it can help identify who might benefit from closer follow-up.”
— Summary of findings from recent European Heart Journal research on mammography and heart risk
What This Means for You (Without the Hype)
It’s tempting to jump straight to, “My next mammogram will tell me if I’ll have a heart attack.” That’s not what this research shows. Instead, here’s a grounded way to think about it:
- It’s a risk signal, not a diagnosis. Finding arterial calcification suggests higher cardiovascular risk, but it doesn’t confirm blocked arteries or guarantee a future event.
- It’s one piece of a larger puzzle. Your age, family history, blood pressure, cholesterol, smoking status, blood sugar, and lifestyle still matter immensely.
- It may get you earlier attention. For some women, this could be the first clue that prompts a real conversation about heart risk and, when appropriate, further testing.
One cardiologist interviewed about this research noted that many women see an OB-GYN far more regularly than a heart specialist. If mammograms can flag heart risk, gynecologists could play a much bigger role in early cardiovascular prevention.
A Realistic Scenario: When a Mammogram Sparks a Heart Check
Consider a composite example based on how this might play out in practice:
Maria, 54, goes for her routine mammogram. She feels generally well, has slightly elevated blood pressure, and a strong family history of breast cancer—but she’s never thought much about heart disease. Her clinic is part of a pilot program using AI to analyze mammograms for arterial calcification.
The AI flags moderate breast arterial calcification. Her radiology report includes a note suggesting that she may be at increased cardiovascular risk and recommends discussing the finding with her primary care clinician.
- Her doctor reviews the finding and orders a cholesterol panel and a more detailed heart risk assessment.
- They discover that her LDL (“bad”) cholesterol is higher than expected and her calculated 10-year risk is moderate.
- Together, they agree on a plan: more consistent exercise, a Mediterranean-style eating pattern, and, after discussion, a low-dose statin medication.
Nothing dramatic happens overnight. But over the next decade, this earlier course correction may lower her chance of a serious heart event. This is the real power of early risk detection: quiet, steady prevention, not miraculous overnight cures.
What to Ask at Your Next Mammogram or Checkup
You don’t need to wait for nationwide AI rollouts to start using your mammogram as a springboard for heart-health conversations. Here are practical, respectful questions you can bring to your next visit:
- “Does your imaging center report breast arterial calcification?”
Some radiologists already note arterial calcification in reports, even without advanced AI. If they see it, ask that this information be shared with your primary care clinician or cardiologist.
- “Given my age and history, should I have a formal heart risk assessment?”
This can include tools like the pooled cohort equations or QRISK (depending on your country) to estimate 10-year cardiovascular risk.
- “Would a coronary artery calcium (CAC) scan make sense for me?”
A CAC scan is a low-dose CT scan that directly measures calcium in heart arteries. It’s not for everyone, but it can be helpful when the decision to start a medication like a statin is uncertain.
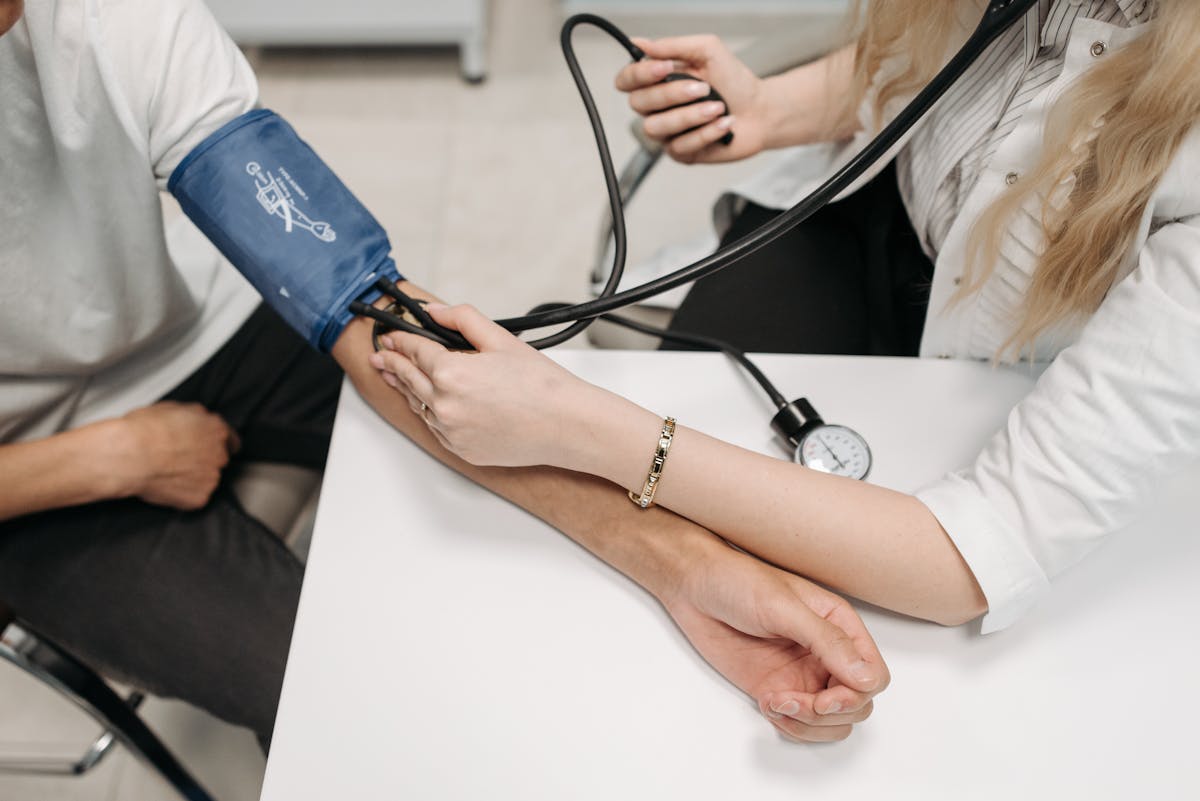
- “Can we review my blood pressure, cholesterol, blood sugar, and weight trends together?”
Mammogram findings should always be interpreted in this broader context, not in isolation.
Common Concerns and How to Navigate Them
It’s completely normal to feel uneasy when technology promises “more” from your tests—more information, more predictions, sometimes more worry. Here are a few common concerns and balanced ways to approach them:
- “Will this just make me more anxious?”
It could, especially if results are presented without context. You can protect yourself by asking your clinician to explain any finding in plain language and to focus on what you can do, not just what might happen.
- “Is AI really accurate and fair?”
Many AI tools perform well in research settings, but they can be influenced by the data they’re trained on. Ask whether the AI used in your setting has been validated in diverse populations, including women of your age, race, and body type.
- “Will this replace my doctor?”
No. In responsible systems, AI is an assistant, not a decision-maker. It can highlight patterns human eyes might miss, but a trained clinician should always interpret and contextualize your results.
From Information to Action: Protecting Your Heart Starting Now
Whether or not your mammogram ever includes an AI-based heart assessment, the core strategies for lowering heart disease risk remain reassuringly familiar—and powerful. Evidence consistently supports these steps:
- Move your body most days. Aim for at least 150 minutes per week of moderate activity (like brisk walking) or 75 minutes of more vigorous exercise, plus two days of strength work. Even short 5–10 minute walks across the day add up.
- Prioritize a heart-healthy eating pattern. Mediterranean-style or DASH-style approaches—rich in vegetables, fruits, whole grains, beans, nuts, olive oil, and fish—are well-studied for cardiovascular protection.
- Know your numbers. At least every 1–2 years (or as advised), track your blood pressure, fasting glucose or A1c (if at risk for diabetes), and a lipid panel (cholesterol profile).
- Don’t ignore sleep and stress. Poor sleep and chronic stress are linked to high blood pressure, weight gain, and inflammation. Small improvements—like a consistent bedtime or a 10-minute daily wind-down routine—can be meaningful.
- Avoid tobacco and limit alcohol. If you smoke or vape, seeking support to quit is one of the single most impactful heart decisions you can make.

Before and After: How Care Could Change When We Use This Information Well
When mammograms are viewed only as breast cancer tools, a woman’s cardiovascular risk may go unaddressed until symptoms appear. When they’re used as dual-purpose images—carefully and ethically—her care pathway can shift:
| Before | After (Ideal Future Scenario) |
|---|---|
| Mammogram read solely for breast cancer; arterial calcification goes unnoticed or undocumented. | Mammogram read for both breast cancer and arterial calcification; clear note sent to primary care when calcification is present. |
| Heart risk only discussed if the woman raises concerns or has obvious symptoms. | Heart risk becomes a standard part of follow-up when arterial calcification is found, even before symptoms. |
| Opportunities for early lifestyle changes and medications may be missed for years. | Earlier, tailored prevention plans reduce long-term risk in a steady, sustainable way. |
What the Research Says (and What It Doesn’t)
The recent European Heart Journal study and similar work don’t stand alone; they build on years of research linking breast arterial calcification to cardiovascular risk. These studies, often involving tens of thousands of women, have shown that:
- Women with BAC are more likely to have coronary artery disease and higher rates of cardiovascular events over time.
- BAC can add predictive value beyond traditional risk factors in some models.
- AI can help quantify BAC more consistently than manual human scoring in some settings.
However, experts are equally clear about current limitations:
- We still need more data on how acting on BAC findings (for example, starting medications earlier) changes long-term outcomes.
- Not all mammography systems or clinics are equipped to capture or analyze BAC at this level yet.
- Guidelines have not fully standardized how BAC should influence treatment decisions.
Turning a Single Test into a Double Opportunity
The idea that a breast cancer screening could also protect your heart is both surprising and quietly hopeful. It doesn’t mean mammograms are magic, or that AI can see your exact future. But it does mean we may soon have one more way to catch cardiovascular risk earlier—especially in women who might otherwise be overlooked.
You don’t have to wait for perfect technology or universal guidelines to benefit. At your next mammogram or annual visit, you can:
- Ask whether your radiology center notes breast arterial calcification.
- Use the appointment as a prompt to talk about your heart risk, not just your breast health.
- Pair any new information with proven steps: movement, nutrition, sleep, stress care, and—when appropriate—medications.
You deserve health care that sees you as a whole person, not a collection of disconnected organs. Let your mammogram be more than a once-a-year event you endure; let it be one more tool you can use to protect both your breasts and your heart, with calm, informed confidence.

Next step: Add one question about your heart to your calendar reminder for your next mammogram—future you will be glad you did.
