How Portable MRI Is Changing Brain Tumour Surgery in Real Time
Portable MRI: Instant Feedback in the Middle of Brain Tumour Surgery
For decades, brain tumour surgery has demanded a difficult kind of courage from both patients and surgeons: much of the critical decision-making happened without real-time imaging, relying on experience, subtle visual cues, and scans taken before or after the operation. Now, a portable MRI used at London Health Sciences Centre (LHSC) in London, Ontario, is changing that equation, giving neurosurgeons “instant feedback” while they operate on complex tumours deep within the skull.
In a world-first, an LHSC team used this compact MRI device during pituitary tumour surgery, allowing the surgeon to pause mid-procedure, scan the patient right in the operating room, and immediately see whether enough of the tumour had been removed. The technology is being hailed as a potential game-changer for brain tumour surgery, with the promise of safer operations, fewer surprises, and less need for repeat procedures.

“Being able to see updated MRI images in the middle of surgery fundamentally changes how we plan and adapt in real time,” the LHSC neurosurgeon explained. “It gives us a level of confidence we simply didn’t have before.”
The Challenge: Brain Tumour Surgery Without Real-Time Imaging
Brain and pituitary tumour surgeries are among the most delicate procedures in medicine. Surgeons operate millimetres away from critical structures responsible for vision, hormones, movement, and memory. Traditionally, they have had to rely on:
- Pre-operative MRI or CT scans taken hours or days before surgery
- Microscopic visualization and neuronavigation systems based on those static images
- Experience and anatomical landmarks to estimate tumour boundaries
Tumours, however, do not always behave predictably. Brain tissue can shift slightly during surgery, and what appears removable on a pre-operative scan may look very different once the skull is opened or the pituitary region is accessed through the nose. This can lead to two major problems:
- Residual tumour: Small but significant portions of tumour may remain undetected until a post-operative MRI is done, sometimes days later.
- Risk to vital structures: Surgeons may stop short of complete removal to avoid damaging critical nerves, blood vessels, or the pituitary gland itself.
What Is a Portable MRI and How Does It Work in the OR?
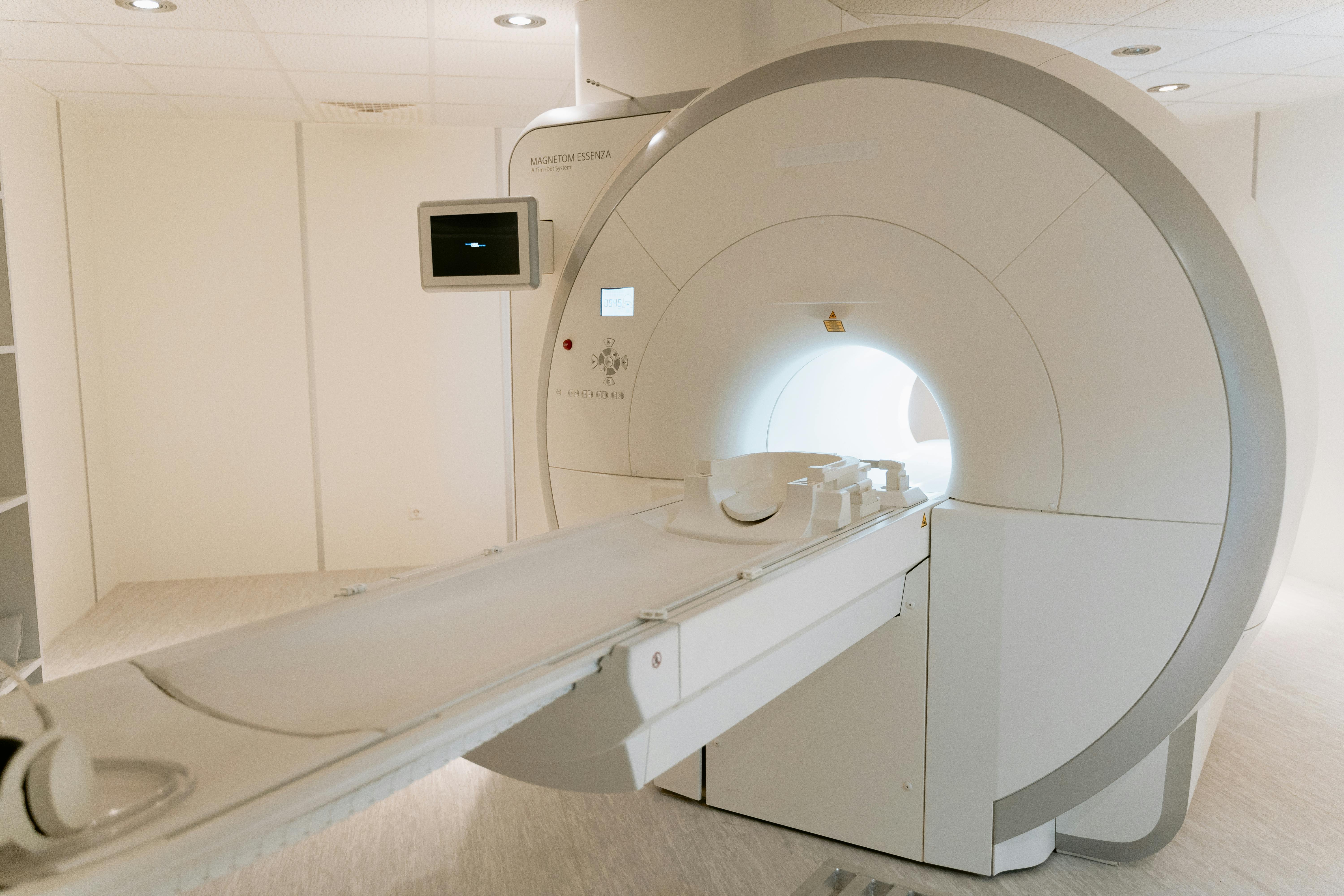
Portable MRI units are compact, lower-field magnetic resonance scanners designed to be brought directly into environments that could never accommodate a traditional MRI suite, such as intensive care units or operating rooms. Instead of transporting a vulnerable post-surgical patient to a separate imaging department, the scanner comes to the bedside or, in this case, the operating table.
In the LHSC case, the team used a portable MRI in the middle of a complex pituitary tumour operation. The process typically involves:
- The surgeon performs the initial phase of tumour removal, often through a minimally invasive approach via the nasal passages.
- The operating field is prepared and secured so that imaging can occur safely and sterile conditions are maintained.
- The portable MRI is brought into the OR and positioned around the patient’s head while they remain under anesthesia.
- A scan is performed, generating images that can be viewed within minutes on screens in the room.
- The surgical team reviews the images to determine whether further tumour removal is needed or whether it is safer to stop.

These devices typically use a lower magnetic field strength than conventional MRI scanners. While this can mean slightly lower resolution, the trade-off is substantial: the ability to see updated images exactly when decisions matter most.
World-First at LHSC: Portable MRI in Pituitary Tumour Surgery
The London Health Sciences Centre team became the first in the world to integrate a portable MRI into pituitary tumour surgery. Pituitary tumours sit at the base of the brain, close to the optic nerves and crucial hormone-regulating structures. Even small residual fragments can cause significant symptoms, including:
- Visual disturbances or loss of peripheral vision
- Headaches and pressure behind the eyes
- Hormonal imbalances affecting growth, fertility, metabolism, and stress response
During this landmark case, the neurosurgeon paused mid-surgery to perform a portable MRI scan. The images revealed how much tumour remained and how close the team was to vital structures. That information allowed them to:
- Decide whether additional tumour tissue could be safely removed
- Avoid over-aggressive dissection that might damage the pituitary gland or optic apparatus
- Reduce the chance the patient would need a second surgery later
“We essentially get to ask, ‘Have we done enough?’ and get an answer in real time,” the surgeon noted. “That’s a profound shift from waiting for a scan hours or days after we’ve already finished.”
Why Portable MRI Is Being Called a “Game-Changer”
While it is early days, clinicians and researchers see several potential benefits from integrating portable MRI into brain tumour surgeries:
- More complete tumour removal when safe: Surgeons can identify residual tumour during the operation and remove additional tissue if it is safe to do so.
- Fewer repeat surgeries: By catching remaining tumour fragments in real time, the need for a second operation may be reduced for some patients.
- Improved protection of critical brain structures: Real-time images can show when the team is “close enough,” helping avoid damage to vital nerves, vessels, and glands.
- Better decision-making under uncertainty: Instead of relying purely on experience and intuition, surgeons can check their impressions against fresh imaging data.
- Greater peace of mind for patients and families: Knowing that the surgical team has access to intraoperative imaging can be reassuring, even though it cannot guarantee specific outcomes.
Before and After Portable MRI: How Surgery Decisions Change
To understand the impact of portable MRI, it can help to compare the traditional workflow with the new approach.
Before Portable MRI
- Surgery is guided by pre-operative scans and navigation systems only.
- Surgeon estimates tumour boundaries and when to stop resection.
- Post-operative MRI is done hours or days later to assess results.
- If significant tumour remains, a second surgery may be scheduled.
With Portable MRI
- Surgery begins as usual, but is paused for an intraoperative scan.
- Fresh images show exactly how much tumour remains.
- The team decides in real time whether to remove more tissue.
- The goal is to leave the OR with a more complete, safer resection.
What This Means if You or a Loved One Has a Brain or Pituitary Tumour
Facing brain or pituitary tumour surgery is overwhelming. It is normal to worry about what surgeons can and cannot see, and whether they will be able to remove “all of it.” Portable MRI does not guarantee a perfect outcome, but it offers a new tool that may improve how those decisions are made.
If you are preparing for surgery, consider asking your neurosurgical team:
- Whether intraoperative or portable MRI is available at your hospital
- How they currently assess the completeness of tumour removal
- What factors might lead them to stop the surgery before removing all visible tumour
- What follow-up imaging and treatments are usually recommended
One pituitary tumour patient described it this way: “Knowing they could check their work right there in the OR didn’t erase my fear, but it made me feel like every possible tool was being used on my side.”
Limitations, Risks, and What We Still Don’t Know
As promising as portable MRI is, it is important to stay grounded about what it can and cannot do. Current limitations include:
- Image resolution: Lower-field portable MRI may not match the fine detail of high-field stationary MRI, which can matter for very small lesions.
- Availability: Only a limited number of centres currently have access to portable MRI technology, and roll-out will likely be gradual.
- Cost and workflow: Integrating a scanner into the operating room is complex and can extend operating time; health systems must balance benefits with resources.
- Evidence base: While intraoperative MRI has shown benefits in some neurosurgical contexts, portable MRI in pituitary and other specific tumour surgeries still requires rigorous long-term study.
There are also safety considerations: MRI requires strict control of metal instruments, implants, and devices. Teams must adapt their workflows and training to ensure that the presence of a magnet in the OR does not introduce new risks.
The Future of Brain Surgery: Smarter, More Adaptive, and More Connected
The LHSC team’s pioneering use of portable MRI in pituitary surgery is part of a broader evolution toward more adaptive, image-guided neurosurgery. Looking ahead, experts anticipate:
- Integration of portable MRI data with advanced neuronavigation and augmented reality displays
- Use of artificial intelligence to help highlight suspicious tissue or measure residual tumour in real time
- Expansion of portable imaging into stroke care, intensive care monitoring, and trauma settings
- Collaborative networks where early-adopting centres share data and protocols to refine best practices

Each of these developments comes with ethical, practical, and economic questions. Ensuring that innovations like portable MRI improve access and outcomes—instead of widening gaps between well-resourced and under-resourced systems—will require careful policy and planning.
Key Takeaways and How to Advocate for Yourself
If you are living with a brain or pituitary tumour, or supporting someone who is, you do not need to be an expert in portable MRI to benefit from this progress. What matters most is informed, collaborative care.
Here are some practical steps you can take:
- Ask about imaging options: Find out if your centre uses intraoperative or portable MRI, and how they decide when to use it.
- Discuss surgical goals clearly: Talk about the balance between maximal tumour removal and preserving function, especially vision and hormones.
- Clarify follow-up plans: Understand what scans and visits you will have after surgery, and what signs should prompt earlier review.
- Seek a second opinion if needed: For complex cases, an opinion from a high-volume centre or academic hospital may give access to newer techniques or clinical trials.
A New Era of “Seeing While Doing” in Brain Tumour Surgery
The first use of a portable MRI during pituitary tumour surgery at London Health Sciences Centre is more than a technical milestone. It represents a shift toward surgeries that are guided not just by what surgeons know before they enter the operating room, but by what they can see and confirm as they work.
Portable MRI will not replace surgical skill, nor will it remove all risk or uncertainty from brain tumour operations. But it adds a powerful new layer of information—one that may help more patients leave the OR with safer, more complete tumour removal and fewer surprises on their post-operative scans.
As this technology spreads and the evidence base grows, staying informed and engaged in your care remains the most important step you can take. If brain or pituitary tumour surgery is on your horizon, consider asking your team how real-time imaging—now and in the future—might support the decisions they make on your behalf.
