The Silent Mold in the Air: How a Shape-Shifting Fungus Became a Global Threat
The deadly fungus in our air: why experts are paying attention now
Imagine breathing in hundreds of invisible spores every single day. Most drift in and out of your lungs without leaving a trace. But some belong to a mold called Aspergillus fumigatus—a microscopic fungus that, in the wrong person, can quite literally “eat you from the inside out.”
Recent reports, including coverage from Earth.com in 2025, highlight how this fungus is spreading and adapting worldwide. It thrives in soil, grains, compost, animal feathers, and even coral skeletons. What makes it especially worrying is how its genome can quickly bend to new pressures such as climate change, pollution, and our own use of antifungal medications.
This doesn’t mean everyone is suddenly at high risk. For most healthy people, these spores are a daily background exposure. But for those with weakened immune systems, lung disease, or frequent hospital stays, Aspergillus can become a life-threatening infection. In this guide, we’ll unpack what the latest science is saying—and more importantly, what you can realistically do to lower risk.
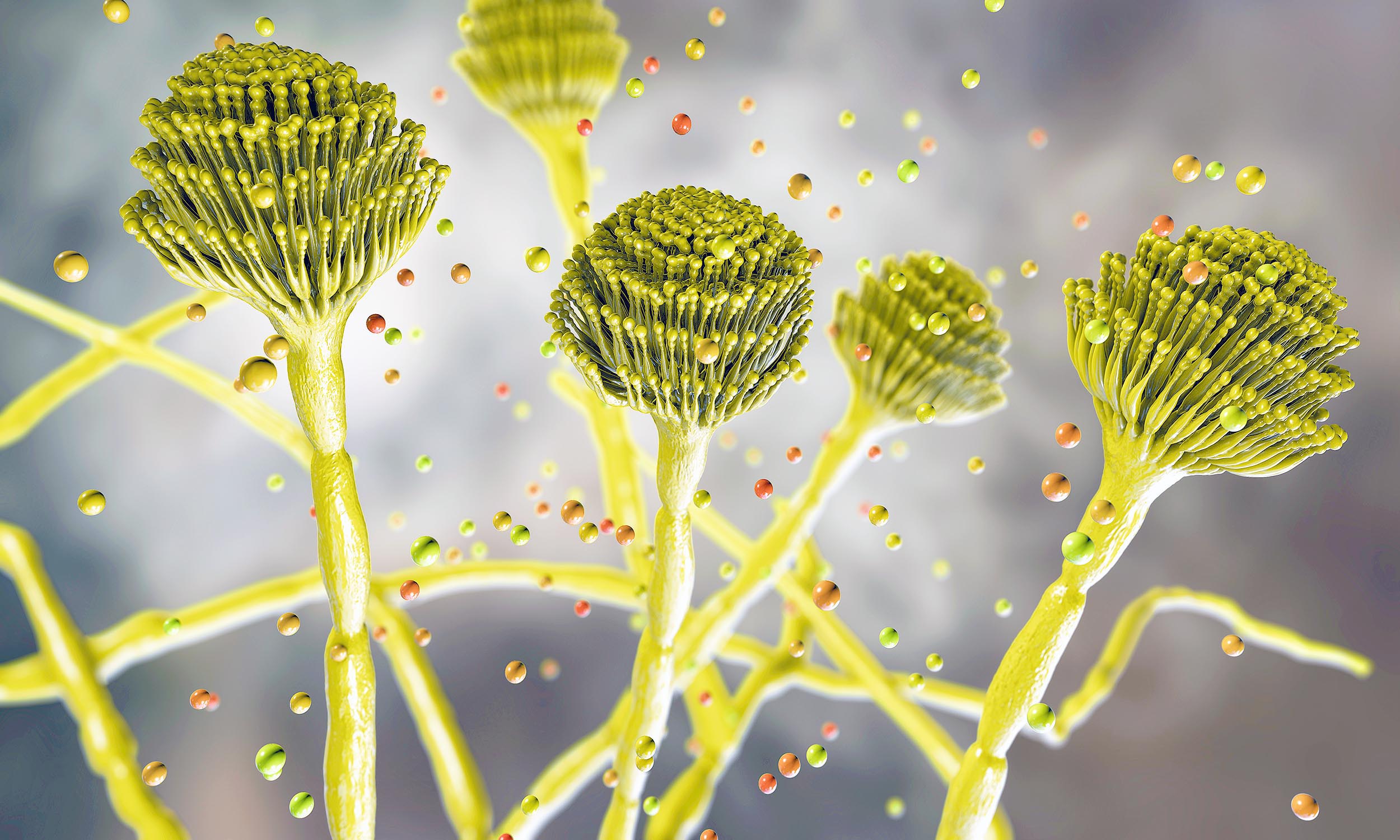
“We are seeing a perfect storm: a highly adaptable fungus, a warming and polluted planet, and a growing population of people whose immune systems are compromised by modern medicine.”
— Infectious disease specialist quoted in recent medical reviews
What is Aspergillus fumigatus and why is it called “deadly”?
Aspergillus fumigatus is a common mold found almost everywhere:
- Soil and compost piles
- Stored grains and decaying vegetation
- Animal bedding and feathers
- Indoor dust, damp building materials, and HVAC systems
You can’t see the spores with the naked eye, and you can’t really avoid them completely. For people with healthy immune systems, these spores are usually filtered and destroyed by the lungs’ defense mechanisms.
The fungus becomes “deadly” when it gets a foothold in someone whose body can’t mount a strong defense. In those cases, it can:
- Colonize the airways, forming clumps of fungal material (sometimes called a “fungus ball”).
- Invade lung tissue, damaging blood vessels and causing bleeding.
- Spread through the bloodstream to organs such as the brain, kidneys, or heart.
This invasive form is why headlines describe it as a fungus that can “eat you from the inside out.” It’s a dramatic phrase—but it reflects how the organism can digest and destroy human tissue when the immune system can’t keep it in check.
How and why is this fungus spreading around the world?
The recent Earth.com feature drew attention to the way Aspergillus fumigatus is spreading and thriving globally. Several interconnected trends are driving this:
1. Climate change and extreme weather
Warmer temperatures and changing rainfall patterns influence where fungi can grow. Research published in the last few years suggests that:
- Hotter, drier conditions in some regions increase dust and airborne spores.
- Flooding and storms promote mold growth indoors as buildings become damp.
- Shifting ecosystems allow fungi to expand into new geographic areas.
2. Global trade, travel, and agriculture
Aspergillus spores can hitchhike on:
- Grain shipments and animal feed
- Compost, plant products, and raw materials
- Clothing, equipment, and even air currents in aircraft
At the same time, large-scale agricultural use of certain azole fungicides (chemicals used to protect crops) is believed to drive the emergence of azole-resistant strains. These resistant strains can then spread through the environment and show up in hospitals, making patients harder to treat.
3. A growing population of vulnerable patients
Modern medicine is a double-edged sword. More people than ever are surviving:
- Cancer and chemotherapy
- Organ and stem cell transplants
- Autoimmune diseases treated with immune-suppressing drugs
These lifesaving treatments also weaken immune defenses, creating a larger group of people who are vulnerable to opportunistic fungi like Aspergillus.

The shape-shifting genome: why Aspergillus adapts so easily
One of the most unsettling details highlighted by Earth.com is that Aspergillus “thrives because its genome bends easily to new pressures.” In more technical terms, this fungus has:
- A relatively compact but flexible genome that can gain or lose pieces of DNA.
- High capacity for mutation and genetic rearrangement.
- Ability to rapidly adjust what genes are turned on or off in response to temperature, chemicals, or immune attacks.
Recent genetic studies have shown that environmental exposure to antifungal chemicals (such as agricultural azoles) can select for mutations that also make the fungus harder to treat in humans. This means the same adaptive power that lets it survive on compost or feathers can also help it:
- Resist medications used in hospitals.
- Withstand higher temperatures, potentially making it more comfortable in the human body.
- Evade immune defenses more effectively.
Who is most at risk from Aspergillus infections?
It’s natural to feel anxious when you hear about a fungus that can cause such severe illness. It’s just as important to remember that risk is not the same for everyone.
Highest-risk groups
- People with profoundly weakened immune systems, such as:
- Recipients of stem cell or solid organ transplants
- Patients receiving intensive chemotherapy for leukemia or lymphoma
- People with advanced or uncontrolled HIV/AIDS (especially with very low CD4 counts)
- Critically ill patients in intensive care units (ICUs), especially those on ventilators or with prolonged hospital stays.
- People on long-term or high-dose corticosteroids or other strong immune-suppressing medications.
Moderate risk groups
- People with chronic lung diseases such as:
- Severe asthma
- COPD (chronic obstructive pulmonary disease)
- Cystic fibrosis
- Prior tuberculosis or structural lung damage
- Individuals with uncontrolled diabetes or other conditions that impair immunity.
Lower risk (but not zero)
Healthy adults and children with normal immune systems and no significant lung disease are generally at low risk of invasive disease. However, they may still:
- Develop allergic reactions to Aspergillus (allergic bronchopulmonary aspergillosis).
- Experience sinus issues or mild respiratory symptoms if living or working in very moldy environments.

“We don’t want the general public to panic about Aspergillus. Our focus is on protecting high-risk patients through better hospital practices, early diagnosis, and smarter use of antifungals.”
— Hospital infectious disease physician, case conference summary
Signs and symptoms to watch for (and when to seek help)
Symptoms of Aspergillus-related disease can vary depending on where the fungus is growing and how strong the immune system is. None of these symptoms are specific to Aspergillus—they overlap with many other conditions—so proper medical evaluation is essential.
Possible symptoms of lung involvement
- Persistent cough that doesn’t improve
- Coughing up blood (even small amounts should be evaluated)
- Shortness of breath or chest tightness
- Unexplained fever, especially in high-risk patients
- Fatigue, weight loss, or night sweats
Allergic or chronic forms
- Worsening asthma symptoms
- Recurring sinus infections, nasal congestion, or facial pain
- Thick mucus plugs or brownish mucus in people with asthma or cystic fibrosis
Urgent medical attention is needed if:
- You are immune-compromised and develop new or worsening respiratory symptoms.
- You cough up blood of any amount.
- You have high fever, chills, or difficulty breathing.
Practical ways to reduce exposure and protect vulnerable people
You can’t sterilize your world—and you don’t need to. But if you or someone you care for is at higher risk, certain targeted, realistic steps can lower exposure and support early detection.
1. Home and indoor environment
- Control moisture:
- Fix leaks and damp areas promptly.
- Use exhaust fans in bathrooms and kitchens.
- Keep indoor humidity ideally between 40–50% with a hygrometer.
- Improve air quality:
- Use HEPA filters in central HVAC or portable air purifiers in main living and sleeping areas.
- Change HVAC filters on schedule (or more often in dusty environments).
- Avoid unfiltered air from heavy construction sites or compost facilities if possible.
- Handle visible mold safely:
- Small patches on non-porous surfaces can often be cleaned with detergent and water while wearing gloves and a mask.
- For extensive growth, water damage, or if someone in the home is immune-compromised, consult professional remediation.
2. Activities to approach with extra care
For high-risk individuals, doctors often recommend limiting exposure to heavily contaminated environments, such as:
- Turning compost piles or working with decaying leaves
- Handling moldy hay, grain, or animal bedding
- Renovation sites with dust and old building materials
If exposure is unavoidable, talk with your medical team about:
- Using an N95 or higher-level respirator
- Leaving high-risk tasks to others when possible
- Ensuring good ventilation and limiting time in the area
3. Hospital and healthcare settings
Many of the most severe Aspergillus infections are acquired or detected while patients are hospitalized. Modern infection control practices include:
- HEPA-filtered rooms for the most vulnerable patients.
- Strict control of construction dust in and around hospitals.
- Protocols for air and surface monitoring in high-risk units.
As a patient or caregiver, you can:
- Ask what air filtration is in place for high-risk rooms.
- Report any visible mold or water damage to staff immediately.
- Discuss with your doctor whether preventive antifungal medication is appropriate for your risk level (never start or stop these on your own).
A real-world scenario: managing fear and risk in an at‑risk family
Several years ago, a lung specialist described a family whose teenage son had just undergone a stem cell transplant. They lived near a large construction site, and the parents were understandably terrified after reading headlines about “deadly airborne fungi.”
Instead of telling them simply “don’t worry” or “you must move,” the care team worked through practical risk-reduction steps:
- The boy spent the highest-risk weeks in a HEPA-filtered hospital room during his most immune-suppressed phase.
- At home, the family:
- Kept windows facing the construction site closed when dust was visible.
- Used a portable HEPA purifier in his bedroom and living area.
- Avoided outdoor walks near the site during peak activity.
- The parents received clear guidance on early warning signs to watch for and a direct line to the transplant team.
This kind of balanced approach—neither denial nor panic—allowed the family to feel some control without placing impossible demands on their lives. It’s a good model for how to live alongside microbial risks in a changing world.
What current research and experts are focusing on
Around the world, scientists and clinicians are working to stay a step ahead of Aspergillus and other invasive fungi. Key areas of focus include:
1. Tracking antifungal resistance
- Surveillance studies to map where azole-resistant Aspergillus strains are emerging.
- Links between agricultural fungicide use and resistance patterns in clinical infections.
2. Better diagnostics and earlier detection
- Improved blood and respiratory tests that can detect Aspergillus before it causes irreversible damage.
- Use of CT scans and biomarkers in high-risk patients to catch invasive disease early.
3. New antifungal drugs and strategies
- Development of novel drug classes aimed at resistant molds.
- Combination therapies and optimized dosing to reduce the development of resistance.
Authoritative organizations such as the U.S. Centers for Disease Control and Prevention (CDC) and the World Health Organization (WHO) regularly update guidance as new data emerges.
At a glance: how Aspergillus exposure becomes disease
Here is a simplified, text-based “infographic” summarizing the path from exposure to potential illness:
- Exposure – You inhale Aspergillus spores from air, dust, soil, or indoor environments.
- Immune defense – In healthy people, immune cells in the lungs destroy spores.
- Risk factors present?
- If no: spores are cleared, often with no symptoms.
- If yes (weak immunity, lung disease, ICU stay, etc.): spores may germinate.
- Colonization or infection
- Allergic response in sensitive individuals (worsening asthma, sinus issues).
- Chronic lung infection with cavities or fungus balls.
- Invasive disease where fungus invades lung tissue and blood vessels.
- Outcome
- Early recognition and treatment can improve survival, especially in invasive disease.
- Delayed diagnosis, strong resistance, or very weak immunity increase the risk of severe outcomes.
Living with invisible fungi: staying alert without living in fear
Aspergillus fumigatus is a powerful reminder that our environment is alive with microbes that are constantly adapting to us—and to the changes we create on this planet. Headlines about a fungus that can “eat you from the inside out” are alarming, but they don’t tell the whole story.
The fuller picture is more balanced:
- Most healthy people coexist with Aspergillus every day without serious illness.
- For vulnerable individuals, it can be life-threatening—and deserves respect and proactive planning.
- We have growing scientific knowledge, better diagnostics, and improving hospital practices to fight back.
If you or someone you love is in a higher-risk group, your next steps might include:
- Talking with your healthcare team about your specific risk level and any recommended precautions.
- Making simple environmental changes at home: moisture control, HEPA filtration where appropriate, and prompt handling of visible mold.
- Learning the early warning signs of infection and when to seek urgent care.
You don’t need to wage war on every microbe in your environment. Instead, focus on protecting the most vulnerable people, supporting your overall health, and staying informed from reliable, science-based sources. That combination—awareness, practicality, and perspective—is your best defense in a world where invisible fungi are here to stay.

If this topic affects you personally—perhaps you’re caring for someone with a weakened immune system—consider starting a simple checklist today: one action for the home, one question for your doctor, and one trusted resource to follow. Small, steady steps can make a meaningful difference.
